eAJKD Poll Results: Undocumented Immigrants and Access to Transplantation
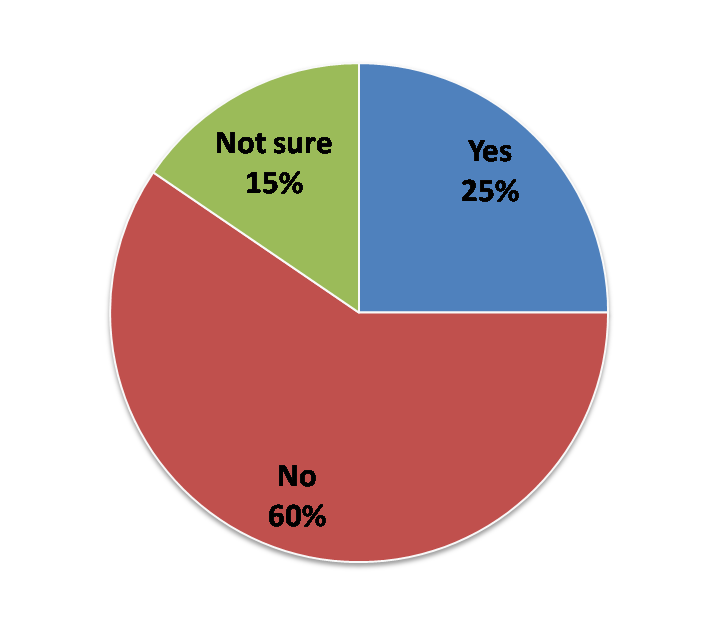
Poll results for the “Should undocumented immigrants get covered for kidney transplantation?” poll.
![]() In the United States, most states are paying for dialysis therapy for undocumented immigrants with end-stage renal disease (ESRD). In a recent study by Linden et al in the September issue of the American Journal of Kidney Diseases, undocumented ESRD patients were found to be healthier than their legal resident counterparts. Although not supported by public policy, many would be ideal candidates for kidney transplantation. It is believed that politics may cloud this policy, and that the nephrology community should facilitate dialogue among stakeholders on this issue. But how does the nephrology community feel about access to transplantation for undocumented immigrants? We set out to answer this question with a poll on eAJKD.
In the United States, most states are paying for dialysis therapy for undocumented immigrants with end-stage renal disease (ESRD). In a recent study by Linden et al in the September issue of the American Journal of Kidney Diseases, undocumented ESRD patients were found to be healthier than their legal resident counterparts. Although not supported by public policy, many would be ideal candidates for kidney transplantation. It is believed that politics may cloud this policy, and that the nephrology community should facilitate dialogue among stakeholders on this issue. But how does the nephrology community feel about access to transplantation for undocumented immigrants? We set out to answer this question with a poll on eAJKD.
Surprisingly, nearly 60% of our readers did not support transplantation in undocumented immigrants, 15% were not sure, and only 25% supported transplantation.
Why won’t the nephrology community support transplantation in undocumented immigrants? The answer seems obvious—at least at first. Transplantation is expensive. Estimates place the first year’s expense to Medicare at about $110,000, with subsequent costs of about $27,000 per year. When there are US citizens who cannot afford transplantation, spending taxpayer money for undocumented patients does not seem appropriate. In addition, transplanting undocumented immigrants takes a kidney away from the deceased donor pool. This may further prolong the wait for others to receive a kidney transplant. Political beliefs on undocumented immigrants may also play a role.
But to make a complete argument, we must consider the benefits of transplanting undocumented immigrants. The price of maintenance dialysis is approximately $75,000 per year. Many undocumented immigrants with ESRD are going to an emergency room for dialysis care, which may be even more expensive. Over the long term, kidney transplantation is cheaper. In addition, transplanting undocumented immigrants may not reduce available organs for citizens. As the study by Linden et al points out, many undocumented patients may have a living donor. Furthermore, although undocumented immigrants do not have access to transplantation, they can still be deceased donors and potentially add to the pool of organs. Finally, not offering transplantation to an otherwise suitable candidate presents an ethical dilemma, as we should be promoting the best treatment options for all of our patients. Unfortunately, there are not many compromises available. One option would be for undocumented immigrants to obtain private health insurance for transplantation, although it may be difficult and expensive. Another option would be to provide access to outpatient dialysis care; although over the long term it will be more expensive than transplantation.
In conclusion, if this poll is representative, the nephrology community does not favor a change in policy to support kidney transplantation in undocumented ESRD patients. Perhaps it is not yet time to discuss policy changes. Rather, we need to first educate ourselves, look hard at data and cost, and come to a consensus as to the best course of action for these vulnerable patients.
Dr. Vinay Nair
eAJKD Advisory Board member

As a legal citizen, I firmly believe that only legal residents should be given dialysis as well as transplantation. We currently have a serious problem with our borders. Our unemployment rate remains high, yet the stream of illegal immigrants continue. The magnet continues as long as unscrupulous employers provide employment to these illegals. They do not provide insurance, just jobs. The taxpayer is burdened whenever these people use the emergency room, encounter law enforcement, etc. Now add dialysis and transplantation to them and the magnet will increase. Our spineless politicians should have had serious discussions with Mexico (as well as other countries) of these illegal immigrants. Mexico currently has a vibrant economy, yet does not care for their own people. Shame on Mexico. Whenever there is a discussion regarding illegal immigration, the country of Mexico is never discussed. Why is that?
I am the grateful recipient of a kidney transplant 7 1/2 years ago. I waited 4 long years, continued to work during this time, provided my own insurance, paid for my medication and co-pays. I continue to work full time in order to care for myself. I resent any immigrant who arrives here expecting to be cared for, I resent any country that does not provide for their own residents. We currently have a deficit in this country unlike any time in the past. Yet you advocate transplantation? NO!
Mary N. Zimmerman