NephMadness 2016: Commentary on BP Measurement—Advantages of Automated BP Monitors
Submit your picks! | For more on NephMadness 2016 | #NephMadness or #HTNRegion on Twitter
Blood pressure (BP) measurement is one of the most commonly performed medical tests in the world. It is a critical measure to determine whether or not a patient is at increased risk for developing atherosclerosis, the main cause of vascular and cerebrovascular diseases. Accurate BP measurement is the foundation of optimal diagnosis and treatment of hypertension.
Blood pressure measurement is commonly performed using a manual technique of auscultation over the brachial artery while observing a mercury sphygmomanometer. This method, developed in 1896 by Riva-Rocci, has not changed appreciably since that time, with the only improvements being auscultation developed by Sergei Korotkoff during the Russo-Japanese War (1904–1905), and Velcro to fasten the cuff.
Manual blood pressure measurements with a calibrated sphygmomanometer can be very accurate, if performed properly. There are, however, widespread concerns about the quality and accuracy of manual blood pressure measurement in routine clinical practice. Some of the problems include the use of uncalibrated sphygmomanometers, inappropriate cuff size, zero-digit bias, patient-clinician interaction during readings, and failure to reduce patient-related factors such as anxiety.
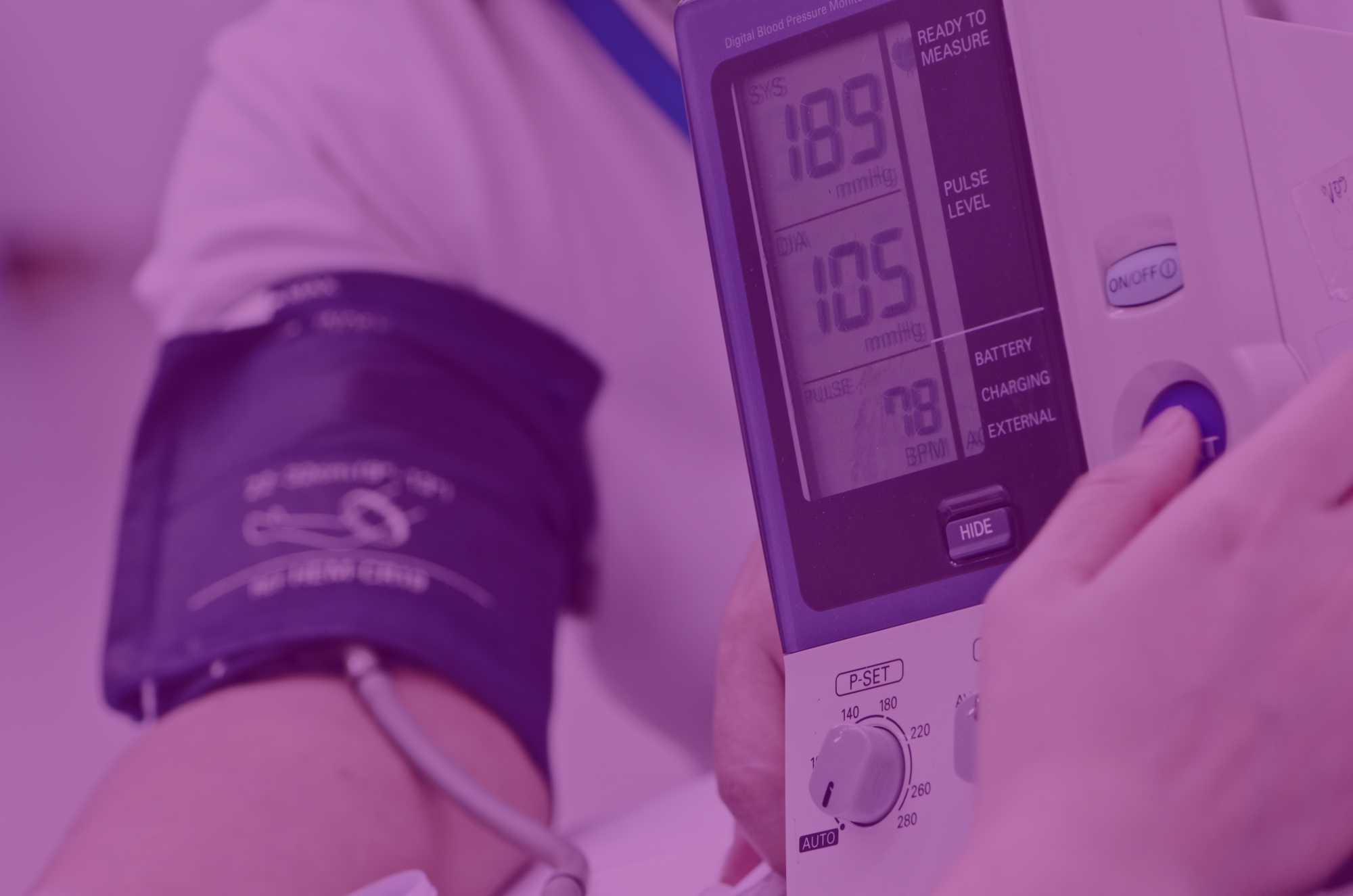
The recent development of fully automated sphygmomanometers, which record multiple BP measurements, offers a possible solution to the problem of inaccurate readings and office-induced hypertension associated with manual readings.
The standardized method for AOBP is to place the patient in the sitting position, with the back supported and the legs resting uncrossed on the ground or on a footstool. A properly fitted cuff is placed on the upper arm, which should rest on a chair arm or table such that the patient’s cuffed upper arm is at heart level. Only cuffs supplied by the manufacturer should be used, as the systems are calibrated as a unit. The clinician should observe the first reading to ensure that it takes a valid BP measurement, and then leave the patient alone in the room to complete the rest of the readings without disturbance or distraction. After instructions are given to the patient, no conversation should take place. The average reading shown on the device should be recorded and used for diagnostic or therapeutic purposes.
When used in this manner, the average BP of multiple measurements in the office or clinic setting has been shown to be very close to the current “Gold Standard” of BP measurement, the average daytime ambulatory BP.
Janusz Kaczorowski, PhD, is a medical sociologist with research background in family medicine, epidemiology, psychology, and sociology. He is Professor and Research Director in the Department of Family and Emergency Medicine at the Université de Montréal. He is a holder of the Dr. Sadok Besrour Chair in Family Medicine and the GlaxoSmithKline-CIHR Chair in Optimal Management of Chronic Disease. He directs the Evaluation, Health Care Systems and Services research theme at CRCHUM research center.
He plays leadership roles in hypertension, stroke, and primary care research communities in Canada. He has an active, collaborative, and multi-disciplinary research agenda that includes optimal use of therapeutics in primary care, primary prevention of cardiovascular disease and stroke, knowledge transfer, health services research, and population health.
He has over 20 years experience in developing, coordinating, and completing all aspects of research studies in primary care. He has held a number of large grants both as principal investigator and co-investigator and has co-authored over 200 peer-reviewed articles.


Leave a Reply