Highlights from the October 2023 Issue
Editor’s Note: We asked authors of Original Investigations to provide short plain-language summaries that would briefly summarize what inspired their study, the basic approach taken, what was learned, and why it matters. We hope our readers will find this valuable in helping them keep up with the latest research in the field of nephrology. Highlights from the October 2023 issue:
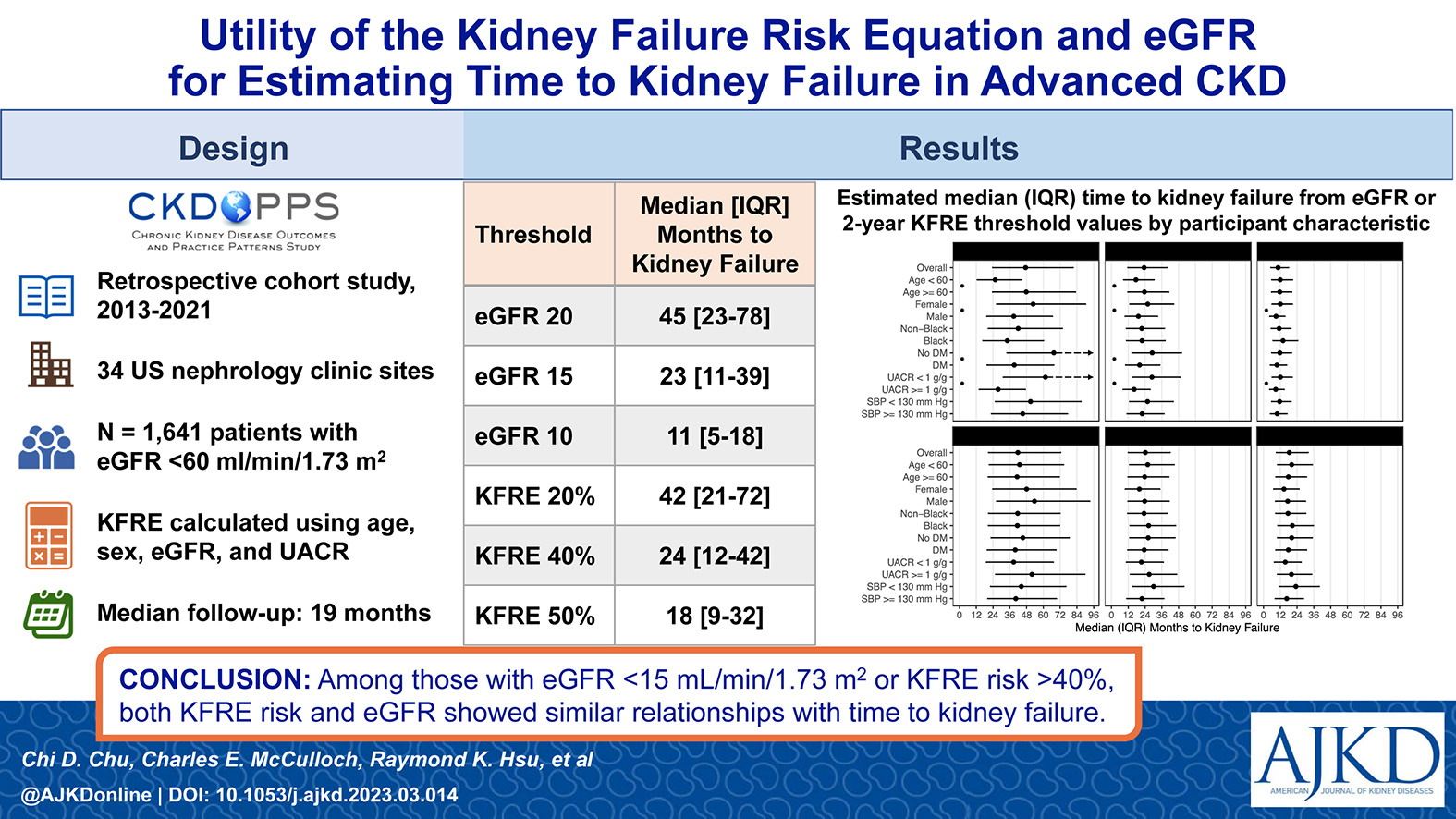
Utility of the Kidney Failure Risk Equation and Estimated GFR for Estimating Time to Kidney Failure in Advanced CKD by Chi D. Chu et al [OPEN ACCESS]
From the authors: Clinicians often talk to patients with advanced chronic kidney disease about the level of kidney function expressed as the estimated glomerular filtration rate (eGFR) and about the risk of developing kidney failure, which can be estimated using the Kidney Failure Risk Equation (KFRE). In a cohort of patients with advanced chronic kidney disease, we examined how eGFR and KFRE risk predictions corresponded to the time patients had until reaching kidney failure. Among those with eGFR < 15 mL/min/1.73 m2 or KFRE risk > 40%), both KFRE risk and eGFR showed similar relationships with time to kidney failure. Estimating time to kidney failure in advanced CKD using either eGFR or KFRE can inform clinical decisions and patient counseling on prognosis.
DOI: 10.1053/j.ajkd.2023.03.014
EDITORIAL: Predicting Kidney Failure With the Kidney Failure Risk Equation: Time to Rethink Probabilities by Roemer J. Janse (FREE)
The Impact of the COVID-19 Pandemic on Patients With CKD: Systematic Review of Qualitative Studies by Patrizia Natale et al
From the authors: During the COVID-19 pandemic, patients with chronic kidney disease (CKD) faced barriers and challenges to accessing care and were at an increased risk of worsened health outcomes. To understand the perspectives about the impact of COVID-19 among patients with CKD and their caregivers, we conducted a systematic review of 34 studies involving 1,962 participants. Our findings demonstrated that uncertainty in accessing care during the COVID-19 pandemic exacerbated the vulnerability, distress, and burden of patients and impaired their abilities for self-management. Optimizing the use of telehealth and providing education and psychosocial services may mitigate the potential consequences for people with CKD during a pandemic.
DOI: 10.1053/j.ajkd.2023.04.001
EDITORIAL: Pandemic Preparedness: Let’s Be Ready for the Patient and Their Caregiver by Suzanne Watnick (FREE)
Kidney Transplantation From Hepatitis C Virus–Infected Donors to Uninfected Recipients: A Systematic Review for the KDIGO 2022 Hepatitis C Clinical Practice Guideline Update by Craig E. Gordon et al [OPEN ACCESS]
From the authors: Due to the high efficacy of direct-acting antivirals (DAA), the use of kidneys from HCV-infected deceased donors may increase rates of kidney transplantation. We conducted a systematic review for the 2022 KDIGO Clinical Practice Guideline on Hepatitis C to evaluate the safety and efficacy of kidney transplantation from HCV-infected donors to uninfected recipients (D+/R−) followed by DAA therapy. Sixteen studies comprising 557 patients revealed high rates of sustained viral response, low rates of adverse events, and excellent patient and allograft survival 1 year after transplantation. Kidney transplantation from HCV-infected deceased donors to uninfected recipients treated with DAA appears safe and effective. Future studies should investigate shorter treatment durations, monitor safety, and obtain longer-term efficacy data.
DOI: 10.1053/j.ajkd.2022.12.019
Patient and Health Care Professional Perspectives on Addressing Obesity in ESKD by Meera Nair Harhay et al
From the authors: Adults with coexisting obesity and end-stage kidney disease (ESKD) are often required to lose weight for kidney transplantation. Yet there is little knowledge about barriers to healthy weight loss in this population. In this study, we conducted interviews with 40 ESKD patients with coexisting obesity and 20 ESKD health care professionals to learn about opportunities to improve obesity-related health care in ESKD. Patients reported that fatigue and dialysis affected dietary choices, and fluid and food restrictions hampered weight loss. Professionals described a lack of training, comfort, and time to address obesity. Patients and professionals reported a lack of open communication about obesity management. Improving obesity-related education and clinical communication should be prioritized to improve care for patients with ESKD and obesity.
DOI: 10.1053/j.ajkd.2023.02.005
Multifaceted Quality Improvement Interventions to Prevent Hemodialysis Catheter–Related Bloodstream Infections: A Systematic Review by Benjamin Lazarus et al
From the authors: People with kidney failure rely on central venous catheters to facilitate life-sustaining hemodialysis treatments. Unfortunately, hemodialysis catheters are a common source of problematic bloodstream infections. Quality improvement programs have effectively prevented catheter-related infections in intensive care units, but it is unclear whether they can be adapted to patients using hemodialysis catheters in the community. In a systematic review that included 21 studies, we found that most quality improvement programs were reported to be successful. However, the findings were mixed among higher-quality studies, and overall the quality of evidence was low. Ongoing quality improvement programs should be complemented by more high-quality research.
DOI: 10.1053/j.ajkd.2023.02.006
Blood Pressure, Incident Cognitive Impairment, and Severity of CKD: Findings From the Chronic Renal Insufficiency Cohort (CRIC) Study by Seda Babroudi et al
From the authors: High blood pressure is a strong risk factor for dementia and cognitive impairment in studies of adults without kidney disease. High blood pressure and cognitive impairment are common in adults with chronic kidney disease (CKD). The impact of blood pressure on the development of future cognitive impairment in patients with CKD remains unclear. We identified the relationship between blood pressure and cognitive impairment in 3,076 adults with CKD. Baseline blood pressure was measured, after which serial cognitive testing was performed over 11 years. Fourteen percent of participants developed cognitive impairment. We found that a higher baseline systolic blood pressure was associated with an increased risk of cognitive impairment. We found that this association was stronger in adults with mild-to-moderate CKD compared with those with advanced CKD.
DOI: 10.1053/j.ajkd.2023.03.012
Perspective from the October 2023 issue:
Magnetic Resonance Imaging to Evaluate Kidney Structure, Function, and Pathology: Moving Toward Clinical Application by Susan T. Francis et al
This Perspective provides an overview of MRI parameters used to assess the kidneys, a review early clinical studies, and a discussion of future developments required to overcome the remaining barriers to clinical application.
DOI: 10.1053/j.ajkd.2023.02.007
 On the Cover: Suzanne Brennan Firstenberg’s installation, “In America: Remember,” blankets the National Mall with a sea of white flags memorializing lives that have been tragically lost to COVID-19. Amid this poignant tribute to those who died, the echoes of the survivor’s struggle also reverberate. In this issue of AJKD, a systematic review of qualitative studies from Natale et al summarizes how the COVID-19 pandemic shaped the health care experiences of patients with kidney disease, including patients with CKD, kidney failure, kidney transplantation, and their caregivers.
On the Cover: Suzanne Brennan Firstenberg’s installation, “In America: Remember,” blankets the National Mall with a sea of white flags memorializing lives that have been tragically lost to COVID-19. Amid this poignant tribute to those who died, the echoes of the survivor’s struggle also reverberate. In this issue of AJKD, a systematic review of qualitative studies from Natale et al summarizes how the COVID-19 pandemic shaped the health care experiences of patients with kidney disease, including patients with CKD, kidney failure, kidney transplantation, and their caregivers.
The photograph “COVID-19 Memorial Field of White Flags 21” by Amaury Laporte is released on Flickr under the CC BY 2.0 license.
Special thanks to Editorial Intern Mengyao Tang for curating the cover image and drafting the cover blurb for this issue
SPECIAL COLLECTION: ACUTE KIDNEY INJURY
This special collection of AJKD articles highlights the latest discoveries in the epidemiology, diagnosis, treatment, and prevention of AKI. All articles are freely available until November 28, 2023.




Leave a Reply