WKD 2018: Kidneys and Women’s Health
Today is World Kidney Day (WKD), a global campaign aimed at raising awareness about kidney health. On its 13th anniversary, the theme for 2018 is “Women and Kidney Disease.” This year, WKD and International Women’s Day are commemorated on the same day, providing a great opportunity to highlight the importance of women’s health and particularly kidney health. The official WKD editorial focuses on what is known and unknown about women’s kidney health and kidney disease, and what we might learn in the future to improve outcomes for all.

AJKD March 2018 cover celebrating World Kidney Day
More than 26 million Americans are affected by chronic kidney disease (CKD), and the prevalence of CKD is increasing. In addition, there is growing evidence that minority populations are disproportionately affected by CKD. African Americans more often have CKD that is more likely to progress to end-stage renal disease (ESRD), compared with whites. Hispanics with CKD also have faster decline in kidney function and increased risk of ESRD, compared with non-Hispanics. People with CKD are at high risk for cardiovascular disease (CVD), and the presence of CKD often complicates cardiovascular (CV) treatment and prognosis. As a result, understanding the relationship of kidney function to CV outcomes within different racial/ethnic groups is of considerable interest.
A 2016 AJKD article by Arce et al coincides with this year’s WKD theme. Using data from the Women’s Health Initiative (WHI), the authors examined the relationship between kidney function and CV events in postmenopausal women of different races/ethnicity. The WHI was a large prospective multicenter cohort study that focused on strategies for preventing heart disease, breast and colorectal cancer, and osteoporotic fractures in postmenopausal women aged 50 to 79 years recruited from September 1993 through December 1998. Arce et al used baseline serum creatinine concentrations of 19,411 postmenopausal women (Figure 1 below) who self-identified as white (n=8921; 46.0%), African American (n=7436; 38.3%), or Hispanic (n=3054; 15.7%) to assess the associations of GFR with myocardial infarction (MI), stroke, and CV death. The authors hypothesized that these associations would differ among racial and ethnic groups.
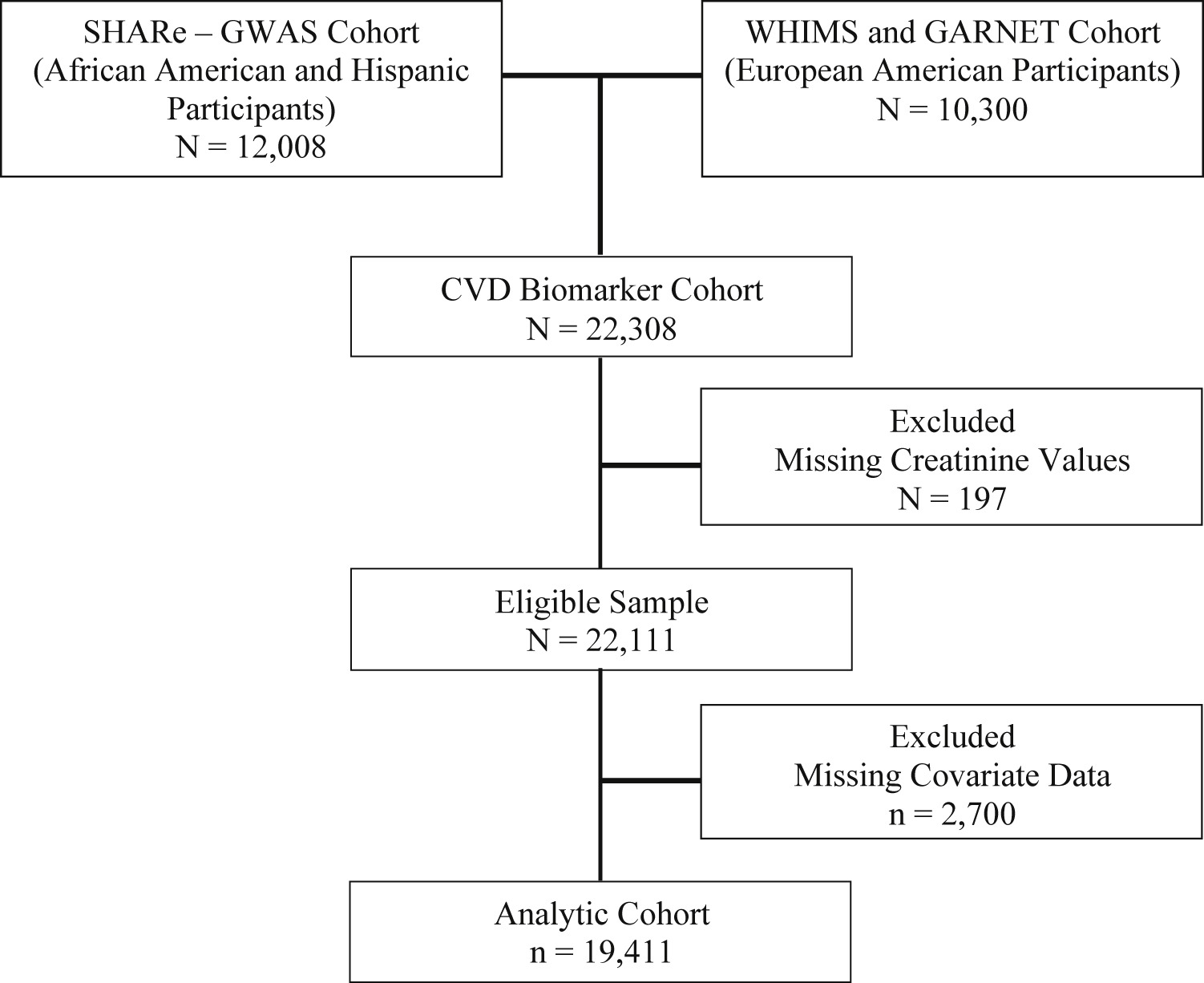
Flow diagram of WHI CVD biomarker study cohort. Figure 1 from Arce et al, AJKD © National Kidney Foundation.
Baseline characteristics of study participants were stratified by eGFR categories and race/ethnicity. Statistically significant differences were noted across racial/ethnic groups for all variables (all P < 0.05). In general, participants with lower eGFRs were more likely to be older, have diabetes, and have a history of MI and stroke. These patients with lower eGFRs were also more likely to have dyslipidemia and higher C-reactive protein levels, regardless of race or ethnicity.
Figure 2 below shows the distribution eGFRs, stratified by self-reported race/ethnicity. In women self-identifying as Hispanic, median eGFR (93.9) was higher than that of whites (85.7) and comparable to that of African Americans (93.7 mL/min/1.73 m2). The range for eGFRs was widest for African American participants and narrowest for white participants.
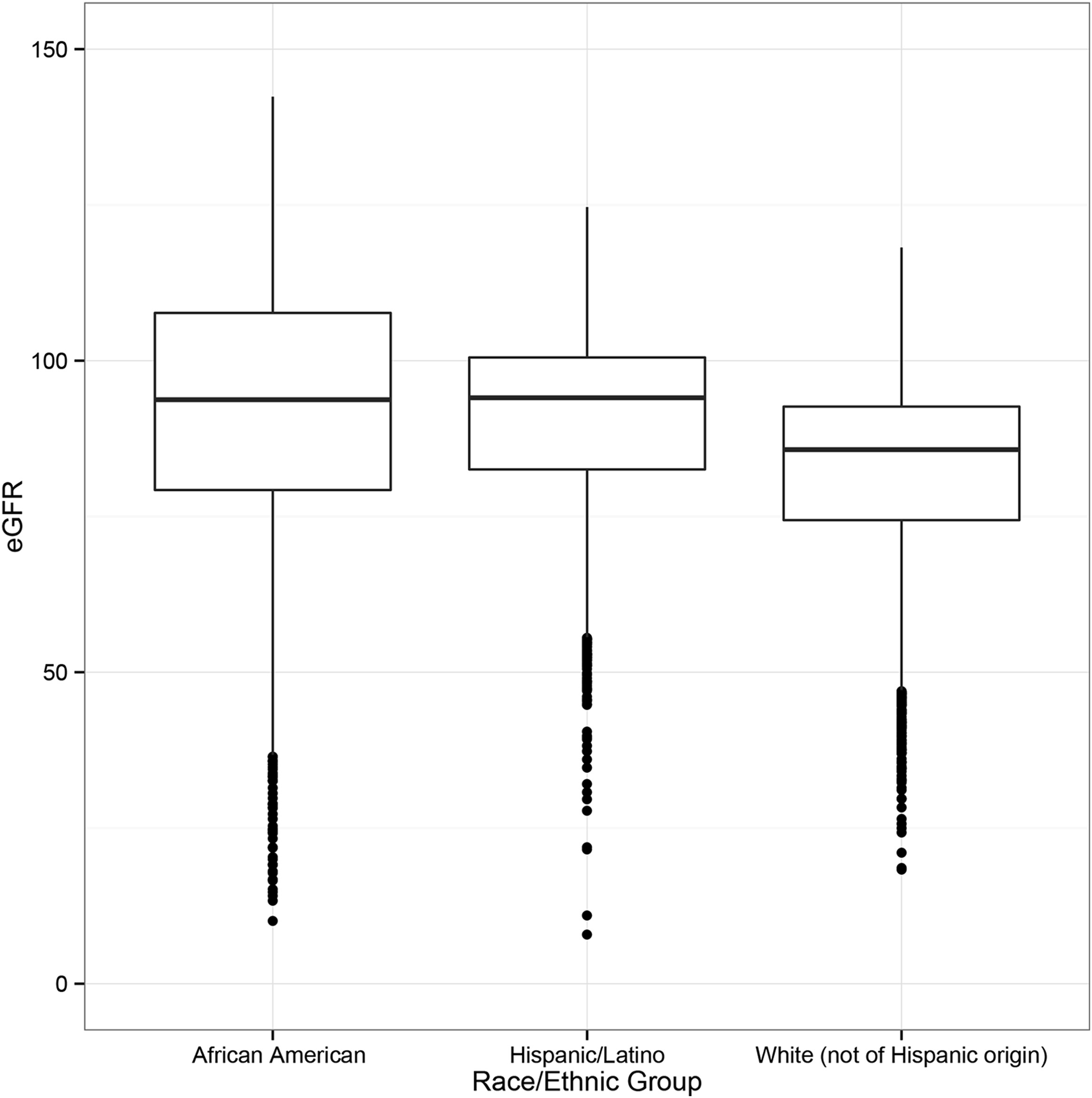
Distribution of estimated glomerular filtration rates (eGFRs; in mL/min/1.73 m2) stratified by self-reported racial/ethnic group. Figure 2 from Arce et al, AJKD © National Kidney Foundation.
Figure 3 below shows adjusted hazard ratios of the composite CV event across categories of eGFR over the 7.6 year mean follow-up stratified by race and ethnicity. The association between eGFR and CV events was curvilinear in the overall cohort; however, the association of eGFR with CV outcomes differed by race (P=.006). Stratum-specific effect modification was found for race (African Americans vs whites, P=.001) but not for ethnicity (Hispanics vs whites, P=.4). Compared to the referent group with eGFRs of 75 to <90 mL/min/1.73 m2, white participants had a U-shaped relationship between eGFR and CV events: both higher (≥105 mL/min/1.73 m2) and lower (<45 mL/min/1.73 m2) eGFRs were associated with higher event rates (HRs of 2.00 and 1.60, respectively). A curvilinear relationship was also observed among African American participants, with lower eGFR being associated with reduced CV risk, and higher eGFR with increased CV risk. Estimates of risk of CV death among Hispanics were inconclusive due to very low or high eGFRs and very few events observed in that group.
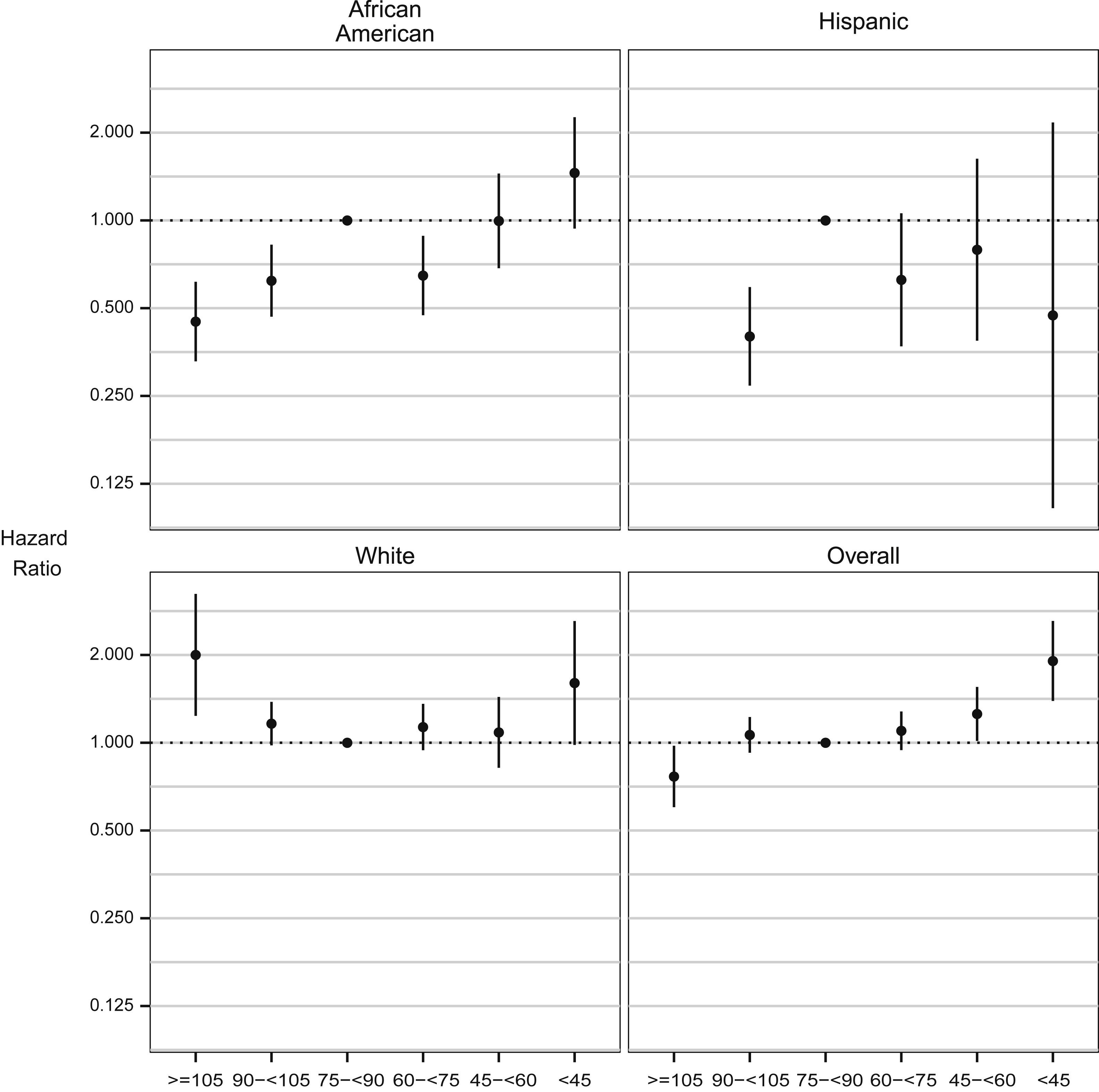
Associations between eGFR and time to CV events (MI, stroke, and CV death); overall and by racial/ethnic group. Figure 3 from Arce et al, AJKD © National Kidney Foundation.
Other studies using the WHI cohort did not find any racial/ethnic differences in CV outcomes in the context of diabetes or obesity. This paper confirms the association of CV outcomes and CKD, as those at highest risk had eGFR <45 ml/min. However, the patterns of association between eGFR and CV outcomes varied between ethnic groups in this paper (compare this to the 2004 landmark study looking at CV risk and kidney disease, where there was a monotonic and linear increase in risk of CV events with progressive decline of eGFR). Interestingly, a novel finding in the WHI cohort was an elevated CV risk with high eGFRs in whites but not in African Americans. This paradox has been reported in the past, and has been attributed to frailty or muscle wasting leading to decreased creatinine generation rather than high levels of kidney function.
These findings encourage future studies to confirm the findings of racially distinct patterns of CV risk from decreased kidney function. Despite study limitations and a cohort of only postmenopausal women, this study and future studies are aligned with sentiments shared in this year’s WKD editorial: “The coinciding of World Kidney Day and International Women’s Day offers an opportunity to develop and define best practices and future research agendas, and ultimately, to optimize outcomes of present and future generations living with or at risk for kidney disease.”
Happy World Kidney Day and International Women’s Day!
– Post prepared by Scherly Leon, AJKDBlog Guest Contributor and NSMC Faculty. Follow her @SLeonMD.
To view Arce et al (FREE until March 31, 2018), please visit AJKD.org.
Title: Kidney Function and Cardiovascular Events in Postmenopausal Women: The Impact of Race and Ethnicity in the Women’s Health Initiative
Authors: C.M. Arce, J.J. Rhee, K.L. Cheung, H. Hedlin, K.Kapphahn, N. Franceschini, R.S. Kalil, L.W. Martin, L. Qi, N.M. Shara, M. Desai, M.L. Stefanick, W.C. Winkelmayer on behalf of the Women’s Health Initiative Investigators
DOI: 10.1053/j.ajkd.2015.07.020

Leave a Reply