Highlights from the February 2021 Issue
Editor’s Note: We asked authors of Original Investigations to provide short plain-language summaries that would briefly summarize what inspired their study, the basic approach taken, what was learned, and why it matters. We hope our readers will find this valuable in helping them keep up with the latest research in the field of nephrology. From the February 2021 issue:
Kidney, Cardiac, and Safety Outcomes Associated With α-Blockers in Patients With CKD: A Population-Based Cohort Study by Gregory L Hundemer et al
From the authors: Alpha-blockers are commonly prescribed as add-on therapy for resistant or refractory hypertension in patients with and without chronic kidney disease. However, the association of α-blocker use, compared with alternative add-on blood pressure–lowering agents, with long-term health outcomes in patients with chronic kidney disease remains unknown. To address this knowledge gap, we compared 16,088 patients in Ontario, Canada, newly prescribed α-blockers to treat high blood pressure with 16,088 matched patients newly prescribed alternative blood pressure–lowering agents. Among patients with chronic kidney disease, α-blocker use was associated with higher risk for kidney disease progression. Conversely, α-blocker use was associated with lower risk for cardiac events and, among patients with reduced kidney function, lower risk for death.
DOI: 10.1053/j.ajkd.2020.07.018
Editorial: Reconsidering α-Blockade for the Management of Hypertension in Patients With CKD by Sarah Ahmad et al [FREE]
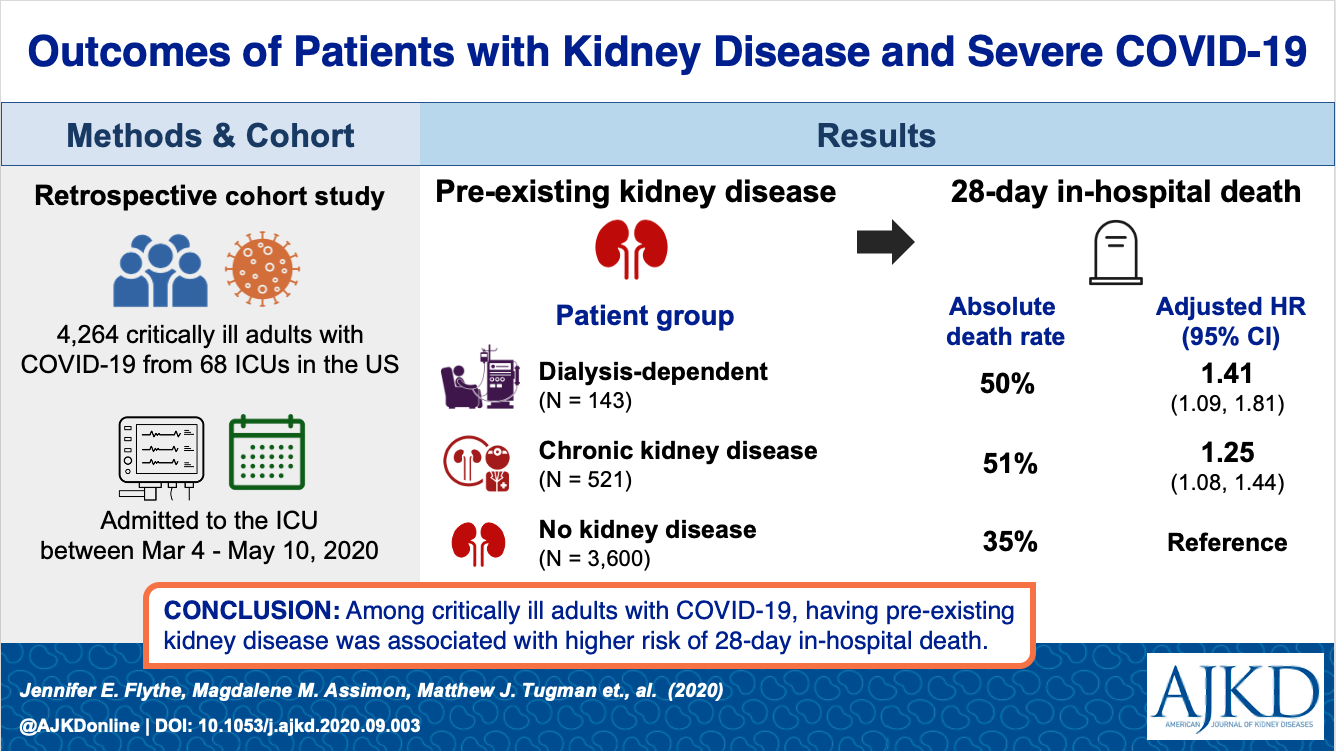
Characteristics and Outcomes of Individuals With Pre-existing Kidney Disease and COVID-19 Admitted to Intensive Care Units in the United States by Jennifer E Flythe et al [FREE]
From the authors: Individuals with underlying kidney disease may be particularly vulnerable to severe coronavirus disease 2019 (COVID-19) illness, marked by multisystem organ failure, thrombosis, and a heightened inflammatory response. Among 4,264 critically ill adults with COVID-19 admitted to 68 intensive care units across the United States, we found that both non-dialysis-dependent chronic kidney disease patients and maintenance dialysis patients had a 28-day in-hospital mortality rate of ~50%. Patients with underlying kidney disease had higher in-hospital mortality than patients without pre-existing kidney disease, with patients receiving maintenance dialysis having the highest risk. As evidenced by differences in symptoms and clinical trajectories, patients with pre-existing kidney disease may have unique susceptibility to COVID-19–related complications, which warrants additional study and special consideration in the pursuit and development of targeted therapies.
DOI: 10.1053/j.ajkd.2020.09.003
Editorial: COVID-19: The Kidneys Tell a Tale by Lili Chan et al [FREE]
Outcomes Among Patients Hospitalized With COVID-19 and Acute Kidney Injury Jia H Ng and Jamie S. Hirsch et al [FREE]
From the authors: In a large New York health system, a significant proportion of patients hospitalized for coronavirus disease 2019 (COVID-19) infection experienced acute kidney injury (AKI), but their overall and kidney-related outcomes were unknown. Given the prolonged hospitalizations for these critically ill patients, studies to date have been hampered by a lack of complete follow-up and outcome ascertainment. We found that the risk for dying in the hospital was significantly higher if one developed AKI and particularly so for those who needed dialytic support. Most patients with AKI who survived to hospital discharge had kidney recovery, although among patients with AKI requiring dialysis, ~31% still needed outpatient dialysis at the time of discharge. Chronic kidney disease was the only independent risk factor associated with requiring dialysis at discharge.
DOI: 10.1053/j.ajkd.2020.09.002
Editorial: COVID-19: The Kidneys Tell a Tale by Lili Chan et al [FREE]
Blog Post An Interview with Jia H Ng [FREE]
Proteinuria Reduction and Kidney Survival in Focal Segmental Glomerulosclerosis by Jonathan P Troost et al
From the authors: Remission of proteinuria has been shown to be associated with a decreased risk for kidney failure in focal segmental glomerulosclerosis (FSGS). This study examined the relationship between changes in proteinuria and progression of kidney disease that occurred in participants of a treatment trial comparing 2 different immunosuppressant regimens. After controlling for other clinical factors, a reduction in proteinuria occurring during the first 26 weeks of treatment was significantly associated with a less steep slope of decline in kidney function measured using estimated glomerular filtration rate and a lower rate of kidney failure or death. These associations were observed even when complete remission of proteinuria was not achieved. These findings provide evidence for the benefit of urinary protein reduction in FSGS. Reductions in proteinuria warrant further evaluation as a surrogate for preservation of kidney function that may inform the design of future clinical trials.
DOI: 10.1053/j.ajkd.2020.04.014
Outcomes Among Patients With Left Ventricular Assist Devices Receiving Maintenance Outpatient Hemodialysis: A Case Series by Douglas D Franz et al
From the authors: Few dialysis centers treat patients with left ventricular assist devices (LVADs) due in large part to a lack of knowledge or experience in performing dialysis for patients on LVAD support outside the hospital. In this case series, we describe 11 patients with LVADs also receiving maintenance outpatient dialysis at Satellite Healthcare. Treatment was guided by specific protocols and with the dialysis unit care team working in close partnership with the LVAD treatment team. Approximately half the patients with complete follow-up either recovered kidney function or underwent combined heart and kidney transplantation. This experience demonstrates that outpatient dialysis can be safely delivered and is well tolerated in patients with LVADs.
DOI: 10.1053/j.ajkd.2020.04.018

LVAD. By Blausen Medical Communications, Inc. See https://commons.wikimedia.org/w/index.php?curid=26986610
Blog Post: The Rise of the LVAD and the Fall of the eGFR: A Commentary on LVAD Patients Receiving Maintenance Dialysis and Rivalry by Natasha Dave [FREE]
Adherence to Healthy Dietary Patterns and Risk of CKD Progression and All-Cause Mortality: Findings From the CRIC (Chronic Renal Insufficiency Cohort) Study by Emily A Hu et al
From the authors: Few studies have been conducted to assess how healthy dietary patterns are associated with chronic kidney disease (CKD) progression among people who have CKD. Therefore, we conducted an analysis among 2,403 people with CKD and examined the associations between their diet quality and risk for CKD progression and all-cause mortality. We found that following a healthy dietary pattern was associated with lower risk for CKD progression and death. These results may inform clinicians to recommend patients with CKD to follow overall healthy dietary patterns that are rich in fruits, vegetables, nuts, legumes, and whole grains and low in red/processed meats, added sugars, and sodium.
DOI: 10.1053/j.ajkd.2020.04.019
International Comparisons of Native Arteriovenous Fistula Patency and Time to Becoming Catheter-Free: Findings From the Dialysis Outcomes and Practice Patterns Study (DOPPS) by Ronald L Pisoni et al [Open Access]
From the authors: Arteriovenous fistulas (AVFs) are the access of first choice, with AVF use greatly differing across countries. However, AVFs are not suitable for all patients. Thus, to maximize patient outcomes and experiences, the goal is to determine the best access for each person, with the current study designed to further inform this goal by describing: (1) international differences in rates and predictors of how long an AVF remains functional (patency), (2) variation in time until first successful AVF use, and (3) outcomes if a new AVF is not successfully used. Our findings highlight the need to reevaluate practices for optimizing achievable AVF outcomes, especially AVF maturation, which was considerably greater in Japan. New AVFs that are not successfully used associate with long-term catheter exposure and substantially higher mortality risk. These findings highlight the importance of selecting the best access type for each patient and developing effective clinical pathways for when AVFs fail to mature successfully.
DOI: 10.1053/j.ajkd.2020.06.020
Policy Forum:
The COVID-19 Pandemic Converges With Kidney Policy Transformation: Implications for CKD Population Health by Sri Lekha Tummalapalli et al [FREE]
From the authors: In this editorial, we outline COVID-19–related payment and regulatory changes and their implications for CKD care delivery and the AAKH Initiative. We then recommend actions for health systems and national professional organizations to achieve optimal equitable CKD population health in the context of COVID-19 and kidney policy transformation.
DOI: 10.1053/j.ajkd.2020.10.004
Blog Post An Interview with Sri Lekha Tummalapalli and Mallika L. Mendu [FREE]
Also from the February 2021 Issue:
KDOQI US Commentary on the 2020 ISPD Practice Recommendations for Prescribing High-Quality Goal-Directed Peritoneal Dialysis by Isaac Teitelbaum et al [FREE]
The recently published 2020 International Society for Peritoneal Dialysis (ISPD) practice recommendations regarding prescription of high-quality goal-directed peritoneal dialysis differ fundamentally from previous guidelines that focused on “adequacy” of dialysis, emphasizing the need for a person-centered approach with shared decision making between the individual performing peritoneal dialysis and the clinical care team while taking a broader view of the various issues faced by that individual. This commentary presents the views of a work group convened by the National Kidney Foundation’s Kidney Disease Outcomes Quality Initiative (KDOQI) to assess these recommendations and assist clinical providers in the United States in interpreting and implementing them. This will require changes to the current clinical paradigm, including greater resource allocation to allow for enhanced services that provide a more holistic and person-centered assessment of the quality of dialysis delivered.
DOI: 10.1053/j.ajkd.2020.09.010
 On the Cover:The Roman mythological bird, caladrius, lifts sickness away from ill human companions by taking it in and flying off to disperse the disease, also curing itself. While ancient notions about medicine were based in mythology, modern medicine emphasizes the importance of evidence from rigorous scientific investigation to drive patient care. The sharing of research surrounding COVID-19 continues at a rapid pace as the global community seeks to understand and control this pandemic using emerging scientific data. In this month’s issue of AJKD, we highlight three articles demonstrating a few of the many ways in which COVID-19 has affected the lives of patients with kidney disease. Flythe et al examine mortality after severe COVID-19 infection among patients with various degrees of pre-existing kidney disease, Ng et al assesses the association between AKI and mortality among patients hospitalized for COVID-19 infection, and Tummalapalli et al explore the implications of the pandemic for CKD population health.
On the Cover:The Roman mythological bird, caladrius, lifts sickness away from ill human companions by taking it in and flying off to disperse the disease, also curing itself. While ancient notions about medicine were based in mythology, modern medicine emphasizes the importance of evidence from rigorous scientific investigation to drive patient care. The sharing of research surrounding COVID-19 continues at a rapid pace as the global community seeks to understand and control this pandemic using emerging scientific data. In this month’s issue of AJKD, we highlight three articles demonstrating a few of the many ways in which COVID-19 has affected the lives of patients with kidney disease. Flythe et al examine mortality after severe COVID-19 infection among patients with various degrees of pre-existing kidney disease, Ng et al assesses the association between AKI and mortality among patients hospitalized for COVID-19 infection, and Tummalapalli et al explore the implications of the pandemic for CKD population health.
Image from the British Library Catalogue of Illuminated Manuscripts available under a CC0 1.0 Universal (CC0 1.0) Public Domain Dedication.
AJKD Express

Recognizing the efficiency losses to authors and reviewers when a manuscript turned down by a high-profile journal is submitted to a new journal, AJKD is excited to offer a new expedited consideration process for manuscripts that meet the following criteria:
- The manuscript reports original research within the scope of AJKD and could be reformatted to AJKD style; and
- The authors supply an unmodified decision letter (including reviews) sent from a high-impact journal within the last 30 days; and
- The author list excludes any AJKD EIC/Deputy Editor/Education Editor/Associate Editor/International Editor.
In this accelerated manuscript consideration process, the editors aim to provide to authors:
- Notification within 2 business days indicating eligibility for AJKD Express
- Decision letter within a further 5-14 days
Details for AJKD Express are available in this blog post.



Leave a Reply