Highlights from the November 2023 Issue
Editor’s Note: We asked authors of Original Investigations to provide short plain-language summaries that would briefly summarize what inspired their study, the basic approach taken, what was learned, and why it matters. We hope our readers will find this valuable in helping them keep up with the latest research in the field of nephrology. Highlights from the November 2023 issue:
The Difference Between Cystatin C– and Creatinine-Based Estimated GFR in Heart Failure With Reduced Ejection Fraction: Insights From PARADIGM-HF by Alberto Pinsino et al
From the authors: Kidney function assessment traditionally relies on serum creatinine (Scr) to establish an estimated glomerular filtration rate (eGFR). However, this has been challenged with the introduction of an alternative marker, cystatin C (cysC). Muscle mass and nutritional status have differential effects on eGFR based on cysC (eGFRcysC) and Scr (eGFRScr). Among ambulatory patients with heart failure enrolled in PARADIGM-HF, we investigated the clinical significance of the difference between eGFRcysC and eGFRScr. More negative values (ie, eGFRScr > eGFRcysC) were associated with worse clinical outcomes (including mortality), poor quality of life, and frailty. In patients with progressive heart failure, which is characterized by muscle loss and poor nutritional status, the decline in kidney function was more pronounced when eGFR was estimated using cysC rather than Scr.
DOI: 10.1053/j.ajkd.2023.03.005
EDITORIAL: Etiologic and Diagnostic Implications of Morbidity and Mortality Associations When Cystatin C–Based Estimated GFR Is Lower Than Creatinine-Based Estimated GFR by Anders O. Grubb (FREE)
Discordances Between Creatinine- and Cystatin C–Based Estimated GFR and Adverse Clinical Outcomes in Routine Clinical Practice by Juan-Jesús Carrero et al (OPEN ACCESS)
From the authors: Clinicians require guidance when there are discrepancies between the estimated glomerular filtration rate based on creatinine (eGFRcr) and based on cystatin C (eGFRcys) in the same individual. Routine cystatin C testing in Sweden for over a decade permits exploration of how common and large these discrepancies are, and their associations with adverse clinical outcomes. In this observational study, we found that discordances between eGFRcys and eGFRcr are common, and 1 in 4 patients tested had an eGFRcys > 28% lower than their eGFRcr. We also show that an eGFRcys that is lower than the eGFRcr consistently identifies patients at higher risk of adverse outcomes, including cardiovascular events, kidney replacement therapy, acute kidney injury, and death.
DOI: 10.1053/j.ajkd.2023.04.002
EDITORIAL: Etiologic and Diagnostic Implications of Morbidity and Mortality Associations When Cystatin C–Based Estimated GFR Is Lower Than Creatinine-Based Estimated GFR by Anders O. Grubb (FREE)
BLOG POST: Cystatin-C- and Cr-Based eGFRs: What Differences Does the Difference Make? An Interview with the Authors (FREE)
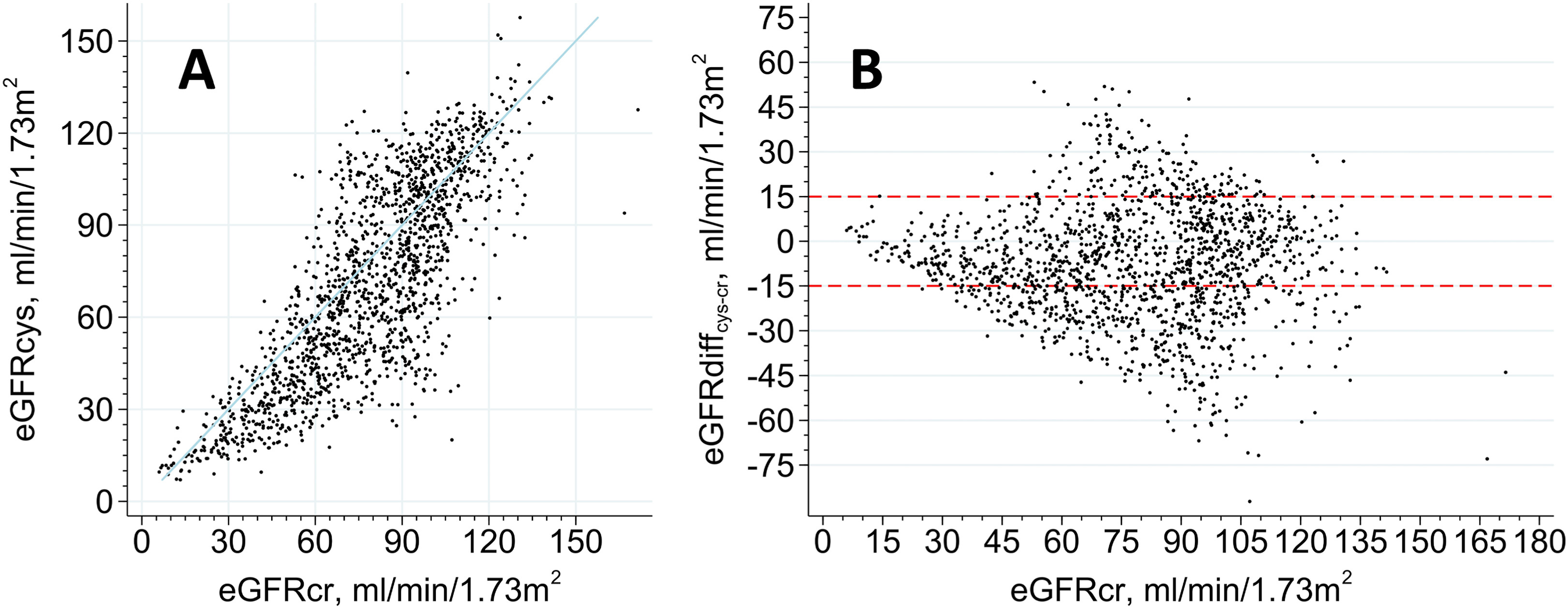
(A) Univariate correlation between eGFRcys and eGFRcr, and (B) scatterplot of eGFRcr versus eGFRdiff at baseline. Shown are correlations in a random 1% sample of 1,569 observations. The blue line shows the line of identity, and red line marks eGFRdiff higher and lower than 15 mL/min/1.73 m2. Figure 1 from Carrero et al, © 2023, the authors.
Vitamin D Therapy in Adults With CKD: A Systematic Review and Meta-analysis by Wing-Chi G. Yeung et al
From the authors: Chronic kidney disease (CKD) is associated with increased risk of death, cardiovascular disease, and fractures. This excess risk is thought to be related to changes in bone and mineral metabolism, leading to the development of CKD–mineral and bone disorder (CKD-MBD) which is characterized by vascular calcification and reduced bone quality. Vitamin D is commonly used in the treatment of this condition. We reviewed randomized controlled trials examining the effect of vitamin D therapy in CKD. We found that vitamin D therapy affects serum biomarkers, including an increase in serum calcium. However, it probably has no effect on risk of all-cause death in CKD, and the effects on other clinical bone, cardiovascular, and kidney outcomes are uncertain.
DOI: 10.1053/j.ajkd.2023.04.003
EDITORIAL: Vitamin D in CKD: An Unfinished Story by Simon Hsu (FREE)

BLOG POST: Vitamin D and Kidney Disease: An Interview An Interview with Dr Yeung (FREE)
Association of Longitudinal B-Type Natriuretic Peptide Monitoring With Kidney Failure in Patients With CKD: A Cohort Study by Tatsufumi Oka et al
From the authors: Both volume overload and volume depletion are deleterious to kidney function. B-type natriuretic peptide (BNP) is a biomarker that reflects volume status not only in heart failure but also in nondialysis chronic kidney disease (CKD). Although longitudinal BNP monitoring may aid physicians’ decision-making about the optimization of volume status, its clinical benefit remains uncertain in CKD. In this cohort study analyzing 2,998 patients with nondialyzed CKD, BNP monitoring was associated with a lower risk of kidney replacement therapy, acute kidney injury, and heart failure hospitalization over the follow-up period. The association with kidney replacement therapy may be mediated through a reduced risk of acute kidney injury or heart failure hospitalization. BNP monitoring may aid physicians in optimal fluid management, potentially conferring better kidney outcomes.
DOI: 10.1053/j.ajkd.2023.05.003
EDITORIAL: Brain Natriuretic Peptide Monitoring in CKD: Ready for Prime Time? by Alexander J. Kula (FREE)
Association of Primary Kidney Disease Type and Donor Relatedness With Live Donor Kidney Transplant Outcomes: An Analysis of ANZDATA by Dong Yu et al (OPEN ACCESS)
From the authors: There are theoretical concerns that live-donor kidney transplants may be associated with increased risks of kidney disease recurrence and transplant failure due to unmeasurable shared genetic factors between the donor and the recipient. This study analyzed data from the Australia and New Zealand Dialysis and Transplant (ANZDATA) registry and showed that, although disease type was associated with the risk of disease recurrence and transplant failure, donor-relatedness did not impact transplant outcomes. These findings may inform pretransplant counseling and live donor selection.
DOI: 10.1053/j.ajkd.2023.04.004
EDITORIAL: It’s All Relative: Donor-Recipient Relationships, Disease Heritability, and Kidney Transplant Outcomes by S. Ali Husain
Trends in the Incidence of End-Stage Kidney Disease in Type 1 and Type 2 Diabetes in Australia, 2010-2019 by Jedidiah I. Morton et al
From the authors: Previous studies showed an increase in new cases of kidney failure among people with type 2 diabetes, but more recent data have not been available. Here, we report trends in the rate of kidney failure for people with type 2 diabetes from 2010 to 2019 and showed that while more people with type 2 diabetes are developing kidney failure, accounting for the fact that they are also surviving longer (and therefore have a higher chance of kidney failure) the growth in this population is not caused by a higher risk of kidney failure. Nevertheless, more people are getting kidney failure than before, which will impact health care systems for years to come.
DOI: 10.1053/j.ajkd.2023.04.007
Fabry Disease Nephropathy: Histological Changes With Nonclassical Mutations and Genetic Variants of Unknown Significance by Marisa Santostefano et al
DOI: 10.1053/j.ajkd.2023.03.015
Core Curriculum in Nephrology from the November 2023 issue:
Kidney Stone Pathophysiology, Evaluation and Management: Core Curriculum 2023 by Shani Shastri et al
Kidney stone disease, also known as nephrolithiasis or urolithiasis, is a disorder in which urinary solutes precipitate to form aggregates of crystalline material in the urinary space. The incidence of nephrolithiasis has been increasing, and the demographics have been evolving. Once viewed as a limited disease with intermittent exacerbations that are simply managed by urologists, nephrolithiasis is now recognized as a complex condition requiring thorough evaluation and multifaceted care. Kidney stones are frequently manifestations of underlying systemic medical conditions such as the metabolic syndrome, genetic disorders, or endocrinopathies. Analysis of urine chemistries and stone composition provide a window into pathogenesis and direct ancillary studies to uncover underlying diseases. These studies allow providers to devise individualized strategies to limit future stone events. Given its complexity, kidney stone disease is best addressed by a team led by nephrologists and urologists with input from multiple other health professionals including dietitians, endocrinologists, interventional radiologists, and endocrine surgeons. In this installment of AJKD’s Core Curriculum in Nephrology, the authors provide a case-based overview of nephrolithiasis, divided by the individual stone types. The reader will gain a pragmatic understanding of the pathophysiology, evaluation, and management of this condition.
DOI: 10.1053/j.ajkd.2023.03.017
 On the Cover: Salmon, along with other fatty fish, is an excellent source of vitamin D. One 310-gram salmon fillet contains 1,630 IU of vitamin D, a level more than twice the daily recommended intake. In this issue of AJKD, Yeung et al conducted a systematic review of randomized controlled trials to evaluate the effect of vitamin D therapy on mortality, cardiovascular, bone, and kidney outcomes in adults with chronic kidney disease. The authors concluded that vitamin D therapy does not reduce the risk of all-cause death. The effects of vitamin D therapy on bone fracture, cardiovascular outcomes, and kidney outcomes remain uncertain.
On the Cover: Salmon, along with other fatty fish, is an excellent source of vitamin D. One 310-gram salmon fillet contains 1,630 IU of vitamin D, a level more than twice the daily recommended intake. In this issue of AJKD, Yeung et al conducted a systematic review of randomized controlled trials to evaluate the effect of vitamin D therapy on mortality, cardiovascular, bone, and kidney outcomes in adults with chronic kidney disease. The authors concluded that vitamin D therapy does not reduce the risk of all-cause death. The effects of vitamin D therapy on bone fracture, cardiovascular outcomes, and kidney outcomes remain uncertain.
The photograph “Salmon” by Michael Saechang is released on Flickr under the CC BY-SA 2.0 license.
Special thanks to Editorial Intern Seolhyun Lee for curating the cover image and drafting the cover blurb for this issue.
SPECIAL COLLECTION: ACUTE KIDNEY INJURY
This special collection of AJKD articles highlights the latest discoveries in the epidemiology, diagnosis, treatment, and prevention of AKI. All articles are freely available until November 28, 2023.


Leave a Reply