Highlights from the February 2026 Issue
Editor’s Note: We asked authors of Original Investigations to provide short plain-language summaries that would briefly summarize what inspired their study, the basic approach taken, what was learned, and why it matters. We hope our readers will find this valuable in helping them keep up with the latest research in the field of nephrology.
Highlights from the February 2026 issue:
Health-Related Quality of Life After Living Kidney Donation: A Systematic Review and Meta-Analysis by Stijn C. van de Laar et al. [OPEN ACCESS]
DOI: 10.1053/j.ajkd.2025.09.008
EDITORIAL: Health-Related Quality of Life After Living Kidney Donation: Insights From a Contemporary Meta-Analysis by Neetika Garg et al. [FREE]
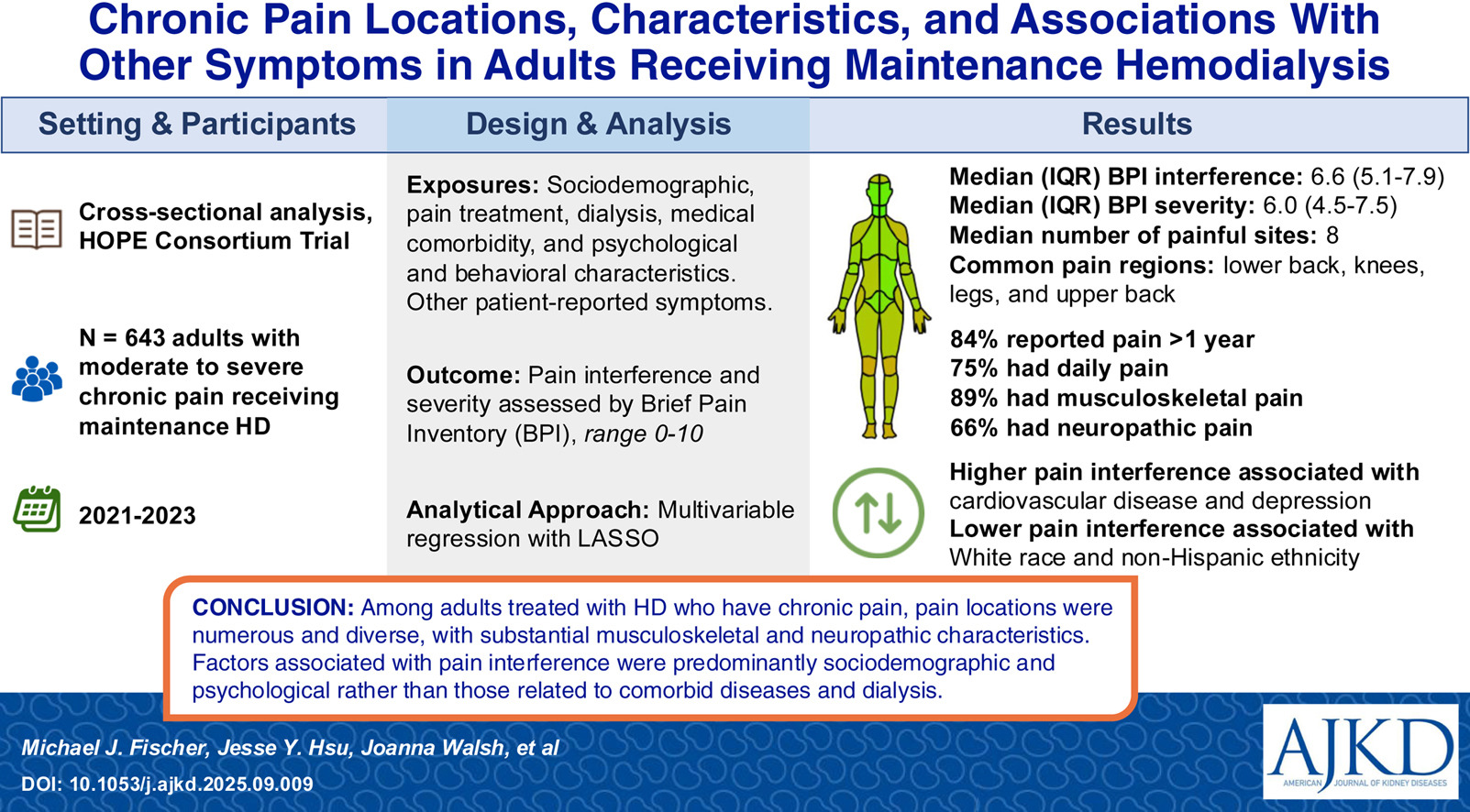
Chronic Pain Locations, Characteristics, and Associations With Other Symptoms in Adults Receiving Maintenance Hemodialysis: Findings From the HOPE Consortium Trial by Michael J. Fischer et al. [OPEN ACCESS]
From the authors: Adults receiving maintenance hemodialysis (HD) frequently experience chronic pain, but it remains poorly understood. We examined pain locations, characteristics, and relationships with other symptoms among 643 adults with moderate to severe chronic pain receiving maintenance HD enrolled in the multicenter HOPE Consortium Trial from 2021 to 2023. We found that pain locations were numerous and diverse, with substantial musculoskeletal and neuropathic pain characteristics. The factors associated with pain interference were predominantly sociodemographic and psychological rather than related to comorbid diseases and dialysis. Given these findings, routine pain assessments and treatment plans tailored to the specific needs and symptoms of the individual patient seem warranted for this patient population.
DOI: 10.1053/j.ajkd.2025.09.009
EDITORIAL: Chronic Pain in Hemodialysis: Beyond the Biochemical Paradigm by James Burton and Katherine Hull [FREE]
Access to Kidney Transplantation in Adults With Severe Obesity: A Population-Based Retrospective Cohort Study by Natasha Wiebe et al. [OPEN ACCESS]
From the Authors: International guidelines do not consider moderate or severe obesity (body mass index ≥35 and ≥40 kg/m2, respectively) to be a contraindication to kidney transplantation, but clinical practice suggests otherwise. Canadian dialysis patients with moderate or severe obesity had a reduced likelihood of receiving a kidney transplant (24% and 57%, respectively). Although patients with moderate or severe obesity also had a heightened risk of allograft failure or death (36% and 70%, respectively), the magnitude of the latter was similar to the excess risk associated with other common clinical characteristics that do not exclude a patient from kidney transplantation. These findings support current practice guidelines and suggest that further work should identify and remove barriers to accessing kidney transplantation among patients with moderate and severe obesity.
DOI: 10.1053/j.ajkd.2025.09.013
Glucagon-like Peptide-1 Receptor Agonists and Risk of Major Adverse Cardiovascular Events in Patients With CKD by Kevin Yau et al. [OPEN ACCESS]
From the authors: A class of medications called glucagon-like peptide-1 receptor agonists (GLP1-RA) is now used for the treatment of diabetes. This study explored the association of GLP1-RA administration with cardiac health in people with kidney disease compared with another common class of diabetes medication, dipeptidyl peptidase-4 (DPP-4) inhibitors. In this study of nearly 69,000 individuals in Ontario, Canada, with a wide range of kidney function, people taking GLP1-RA experienced a lower rate of heart disease than those taking DPP-4 inhibitors. The lower rate was mainly related to fewer deaths from heart disease. Differences were consistent across different levels of kidney disease and regardless of whether people were also taking other medications that protect the heart.
DOI: 10.1053/j.ajkd.2025.09.010
Core Curriculum In Nephrology in the February 2026 issue:
Exercise and Kidney Health: Core Curriculum 2026 by Laura Aponte Becerra and Sherry Mansour [OPEN ACCESS]
DOI: 10.1053/j.ajkd.2025.09.014
AJKD is honored to host the 14th annual NephMadness, organized by Executive Team members Matthew Sparks, Anna Burgner, Anna Vinnikova, Samira Farouk, Jeffrey Kott, Ana Catalina Alvarez-Elas, Dia Waguespack, and Krithika Mohan. This educational initiative highlights 8 important nephrology topics and encourages participants to select the one most likely to change kidney disease care in the next 5 years. US-based physicians can claim up to 8.0 CME credits for this activity. The fun and learning will begin on March 1, 2026, at AJKDblog.org.
The NephMadness 2026 logo is created by Graham T. Gipson.
Call for Applications: AJKD Editorial Internship Program 2026-27
 The AJKD Editorial Internship Program provides editorial experience to early career researchers interested in education, teaching, or medical editing/writing. Apply by April 30, 2025. Details on the AJKD Blog.
The AJKD Editorial Internship Program provides editorial experience to early career researchers interested in education, teaching, or medical editing/writing. Apply by April 30, 2025. Details on the AJKD Blog.



Leave a Reply