#NephMadness 2020: Ethics Region
Submit your picks! | NephMadness 2020 | #NephMadness | #EthicsRegion
Selection Committee Member: Amaka Eneanya @AmakaEMD
Amaka Eneanya is an Assistant Professor of Medicine and attending nephrologist at the University of Pennsylvania. She is an NIH-funded clinical investigator with research interests that include improving palliative care access, informed decision-making, and racial disparities among patients with advanced chronic and end-stage kidney disease.
Writer: Devika Nair @devimol
Devika Nair is an Instructor of Medicine in the Division of Nephrology and Hypertension at Vanderbilt University Medical Center. Her research focuses on using qualitative and quantitative methods to better characterize and intervene on mood disorders in patients with advanced kidney disease. She was a member of the inaugural class of AJKD Editorial Interns.
Competitors for the Ethics Region:
Policy-Driven Outcomes for Dialysis vs Patient-Driven Choice for Dialysis
End-of-Life Care for Patients on Dialysis vs Dialysis for Patients at End-of-Life

Copyright: Kaspars Grinvalds / Shutterstock
“Until he extends the circle of his compassion to all living things, man will not himself find peace.” ― Albert Schweitzer, MD
Ethics are moral principles that affect how individuals behave and make decisions to benefit themselves or society as a whole. In the context of healthcare, “ethics” refer to the principles, values, and beliefs that inform treatment decisions and policies involved in caring for the ill. In this year’s NephMadness, we highlight timely policy issues in nephrology as they relate to the ethical principles of beneficence, respect for autonomy, nonmaleficence, and justice.
Policy-Driven Outcomes for Dialysis (Beneficence) vs Patient-Driven Choice for Dialysis (Respect for Autonomy)
Policy-Driven Outcomes for Dialysis (Beneficence)
Beneficence is rooted in the moral imperative that our actions must promote collective well-being. The legislative decision in the United States to provide Medicare coverage for individuals with end-stage kidney disease (ESKD) who require kidney replacement therapy was crafted in the spirit of beneficence.
In its infancy, hemodialysis (HD) was only offered to a select group of individuals based on their “social worth”, a highly subjective assessment derived from a combination of demographic and psychosocial factors. With an increasing prevalence of kidney disease, as well as improvements in dialysis technology, patients, physicians, and other stakeholders urged for this life-saving therapy to be made available to all those in need.
As a result of a series of hearings held by the House Ways and Means Committee—including testimony by Belding Scribner (nephrologist at the University of Washington and co-inventor, with Wayne Quinton, of the first vascular access device),William Flanigan (nephrologist at the University of Arkansas), George Schreiner (nephrologist at Georgetown), and a live demonstration of Shep Glazer receiving HD on the House floor—HR Bill 12043 was introduced to provide financial support for patients with kidney disease. After additional legislative hearings, the Social Security Amendment of 1972 was passed to extend Medicare coverage to individuals under 65 who required HD or a kidney transplant for kidney failure.
Peritoneal dialysis (PD) was developed prior to HD, and, though its uptake increased between 1978-1993, the use of PD and other home modalities has steadily declined ever since. Between 2001-2008, the number of individuals with ESKD in the US grew from 294,731 to 383,337. Only 1.4% of this growth represented PD patients, and only 2.4% represented patients on home HD. In 2016, home dialysis accounted for only 8.3% of all patients on dialysis.
Perhaps as a result of this alarming decline, regulatory policies specific to home dialysis have taken center stage in recent US legislation. The ‘Advancing American Kidney Health’ Initiative, introduced in July 2019, aims for 80% of patients with ESKD to obtain a transplant or be maintained on a home dialysis modality (HD or PD) by 2025. This policy-driven healthcare decision brings us to the core of this ethical matchup.
Currently, in-center HD remains the most widely used form of kidney replacement therapy in the US; in 2016, 88% of ESKD patients received dialysis via this modality. This is in contrast with countries such as Hong Kong, Mexico, New Zealand, Colombia, and Qatar, where the prevalence of home modalities such as PD is much higher. Increased uptake of home dialysis therapies is influenced by a number of factors, including physician attitudes and practice patterns, patient health literacy, socioeconomic status, the availability of resources, and system-wide policies.
Policies incentivizing home dialysis in the US would potentially uphold the ethical principle of beneficence on both a national and individual level. The prevalence of ESKD in the US continues to rise, and as a result of the aging population and changes in models for delivery of dialysis, treatment of ESKD incurs a significant economic and clinical burden. Prior budget analyses have demonstrated the possibility of Medicare savings ranging from $114 to $350 million over a five-year period if the percentage of patients on home modalities were to be increased. Patients on PD require lower doses of erythropoiesis stimulating agents to achieve a target hemoglobin level, and Medicare’s expansion of the prospective payment system (PPS) to cover the cost of parenteral medications for each dialysis treatment was a financial incentive for this modality. The cost-effectiveness of home vs in-center modalities has also been demonstrated in analyses of payment models from multiple international health systems.
More importantly, increasing the use of home modalities has the potential to not only decrease economic burden, but also to improve outcomes on an individual patient level. Though data from randomized clinical trials are lacking, home modalities are generally associated with more favorable morbidity and mortality as compared to in-center therapies. PD is linked to better preservation and recovery of residual kidney function, fewer infectious complications, and better preservation of dialysis access. Home HD is associated with improvements in cardiac structure, nutritional parameters, and (potentially) survival. In a recent retrospective cohort study, patients receiving in-center HD reported lower scores on measures of kidney disease-related quality of life across several domains, as compared to those receiving home modalities.

Copyright: CalypsoArt / Shutterstock
If home modalities are associated with decreased economic burden as well as improvements in quality of life, morbidity, and mortality, shouldn’t these therapies be strongly incentivized for any patient who forgoes conservative management?
There is significant discordance between the desire to initiate and maintain patients on PD vs the actual incidence of PD utilization, and many patients are unaware that PD is an option for kidney replacement therapy.
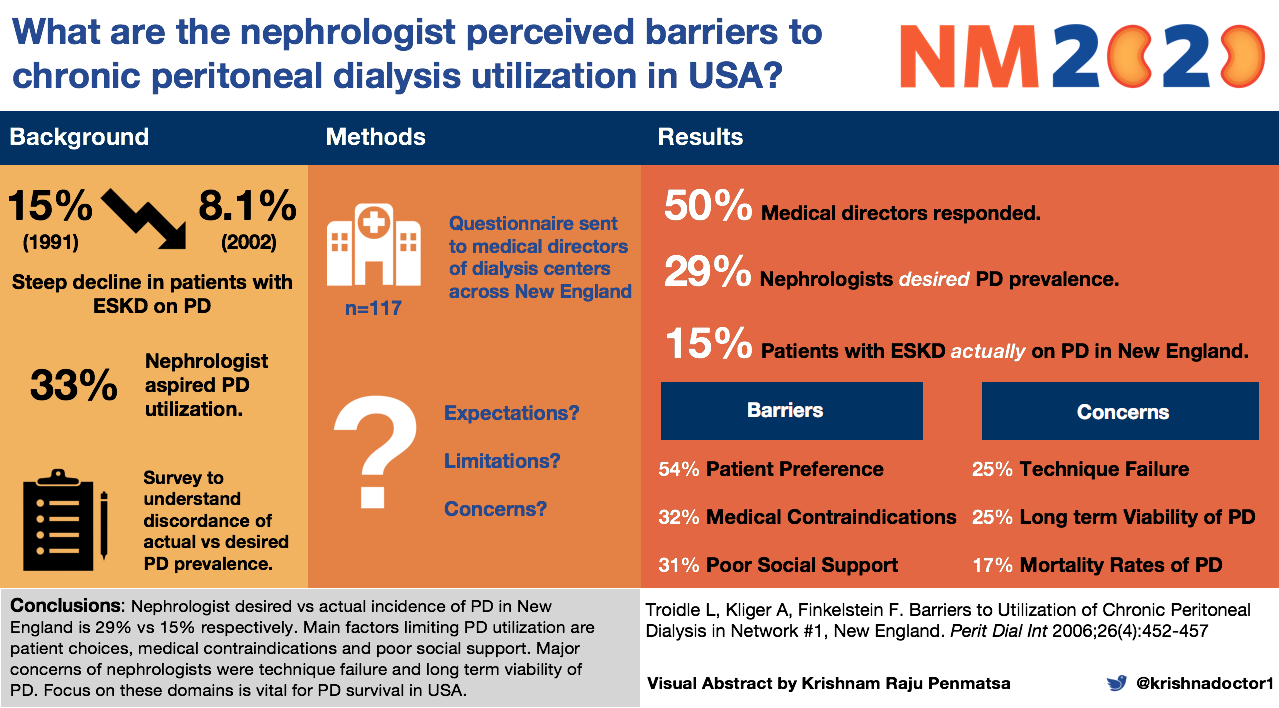
Visual Abstract by @krishnadoctor1 on Troidle et al
Studies have also pointed to potentially modifiable barriers to engagement with home therapies, such as a lack of knowledge and a fear of failure. Targeted educational interventions that actively introduce patients to home modalities are associated with increased odds of choosing and subsequently receiving PD. Initiating a patient on home HD or PD as first-line kidney replacement therapy may also encourage retention into these therapies. Studies show that many patients are reluctant to switch to an alternate modality once an initial choice is made, even if switching were to confer a survival benefit.
Would systems-level policies in the US that incentivize home therapies decrease costs, improve patient outcomes, and ultimately, provide home dialysis to patients who would have otherwise declined or not been offered this therapy?
Recent studies have demonstrated that expansion of the PPS resulted in increases in the incidence and maintenance of individuals receiving PD. Time, observation, and additional analyses of the downstream effects of these new policy changes will be needed to determine if the Advancing American Kidney Health Initiative upholds the ethical principle of beneficence in the long-term.
Patient-Driven Choice for Dialysis (Respect for Autonomy)
Policies incentivizing home dialysis may ultimately uphold beneficence, but they raise other ethical issues related to dialysis decision-making. Beneficence requires understanding that what is good for one patient may not necessarily benefit another.
Incentivizing home modalities is a noble goal, but in crafting policies aimed to provide the greatest benefit to the largest number of people, do we risk sacrificing individual patient autonomy?

Copyright: Lightspring / Shutterstock
Patient autonomy allows for an individual to make decisions in alignment with his or her moral framework, unencumbered by the needs, desires, or perspectives of others. Physicians act to preserve patient autonomy by engaging their patients in shared decision-making. First described by the President’s Commission for the Study of Ethical Problems in Medicine and Biomedical and Behavioral Research, “shared decision-making” is considered the ideal principle on which to model patient-physician interactions. It requires that clinicians provide information, support deliberation, and ultimately reach decisions that align with patients’ values and preferences.
If presented with all available options, would patients be more likely to choose a home dialysis modality?
This question may be impossible to answer. A patient’s decision to choose one dialysis modality over another is influenced by a number of factors. These include, but are not not limited to age, income, desire for travel, functional status, prior history of dialysis, life goals, personal autonomy, cultural beliefs, social support, relationship with the healthcare team, coping styles, presence of comorbid depression or malignancy, and caregiver dependence. For some patients, home dialysis may not be the modality that is most in line with their goals, values, or clinical needs.
There may be individuals (such as those with unstable living situations, poor caregiver support, or comorbid conditions impacting the peritoneum) for whom home therapies could simply be untenable. Additionally, qualitative analyses reveal that caregiver burden may be a concern for many patients who are maintained on home modalities. Will future dialysis facilities be at a financial disadvantage if they care for a larger percentage of patients for whom home modalities may not confer a survival or quality of life benefit? Would they be similarly penalized for providing in-center HD for the majority of their population, even if this is the preferred choice of the patient and their caregivers?
Other countries have changed their policies related to home dialysis to optimize patient autonomy. The 2011 guidelines from the National Institute for Health and Care Excellence (NICE) in the United Kingdom (UK) required that PD be offered as first-line therapy to those with preserved residual kidney function and without significant comorbid conditions. More recent NICE guidelines, however, have prioritized shared decision-making to determine initial modality choice in a manner similar to the recommendations from the Renal Physicians’ Association (RPA).
Putting patients at the center of dialysis decision-making is difficult to argue against, but it is important to remember that patient autonomy in shared decision-making requires that a patient be fully informed of risks and be fully capable of making decisions. In healthcare systems, processes of informed consent are intended to ensure that patients have an adequate understanding of the consequences of a treatment decision. Unfortunately, evidence suggests that patients are not always fully informed of the burdens and risks associated with dialysis and, in retrospect, some may even regret their decision to start dialysis.
Are there patients for whom preserving autonomy may not confer the greatest benefit?
For example, patients with frequent peritonitis may be better suited for in-center HD, but should we instead maintain them on PD if they prefer this modality? Shouldn’t we also assess patients’ self-efficacy and facilitate healthy coping behaviors to better support their treatment decisions before we proclaim “treatment failure”? How can we best respond when a patient, in spite of all ideal resources and support, continues to fare poorly using a specific modality?
Home HD and PD are undoubtedly associated with an improved clinical and symptom profile for many individuals with ESKD, but we must ensure that adhering to these new policy mandates still preserves patient autonomy and engagement in shared decision-making. Although not typically considered an ethical decision for most nephrologists, this policy versus patient matchup should spur dialogue on how these decisions could potentially affect clinical care.
COMMENTARY BY FIONA LOUD:
Decisions, Decisions…A Post About Home Therapies
End-of-Life Care for Patients on Dialysis (Nonmaleficence) vs Dialysis for Patients at End-of-Life (Justice)
End-of-Life Care for Patients on Dialysis (Nonmaleficence)
End-of-life (EOL) care requires that treatment decisions are concordant with an individual’s goals, values, and beliefs. Upholding nonmaleficence in EOL care additionally requires that these decisions inflict little to no harm. A growing body of evidence supports the idea that kidney replacement therapy does not confer a significant survival or quality of life benefit in many older adults with advanced kidney disease. Additionally, patients who receive dialysis experience more intense EOL care and are less likely to use palliative resources such as hospice compared to those who do not receive dialysis.
If we fail to seriously consider conservative management for these patients, are we at risk of violating nonmaleficence?

Copyright: Photographee.eu / Shutterstock
The prospect of withholding dialysis is a decision faced by nephrologists throughout the world. In a survey among US nephrologists, nearly 90% reported having withheld dialysis therapy over the preceding year. In an Australian study of 721 patients with Stage 5 CKD and an average age of 80, 65% were offered conservative care as an initial option. In a Canadian study, roughly 25% of patients referred for dialysis initiation ultimately were not offered the therapy. Do reasons for withholding dialysis differ internationally?
In a study comparing practice patterns of American, British, and Canadian nephrologists, American nephrologists offered dialysis more frequently than their international counterparts, ranking patient/family wishes and fear of litigation as reasons for this. In the same vein, British and Canadian nephrologists more frequently ranked perceptions of their patients’ quality of life as reasons to withhold dialysis. In a qualitative study of 59 nephrologists from the US and UK, barriers and facilitators to to foregoing or withdrawing from dialysis included national policies and structural support for conservative management programs, cultural differences in the practice of medicine, beliefs of patients, the presence or absence of training in goals-of-care conversations, and financial incentives to dialyze.
Withholding dialysis may not always reflect the beliefs and practice patterns of nephrologists, as, in some resource-poor environments, treating advanced CKD with kidney replacement therapy would result in significant economic strain. In the aforementioned survey study, 10% and 12% of Canadian and British nephrologists (as opposed to 2% of American nephrologists) withheld dialysis due to a concern with lack of resources.
Withdrawal of dialysis occurs when the decision is made to suspend the provision of kidney replacement therapy. Apart from cardiovascular and infectious disease-related causes, voluntary dialysis withdrawal is the most common cause of mortality in the US dialysis population. A 1986 study accurately predicted that patient-initiated withdrawal of dialysis would become more frequent in the future, citing the advancing age of patients with ESKD.

Visual Abstract by @MarioFunesMD on Neu et al
In 1989, voluntary dialysis withdrawal constituted 9.7% of ESKD deaths and by 1992, that number rose to 16%. In a 2005 DOPPS analysis, the US had the highest prevalence of dialysis withdrawal as compared to France, Germany, Italy, Japan, Spain, and the UK. In the US, voluntary dialysis withdrawal is more prevalent among those who are women, who self-identify as white, who suffer from coexistent depressive symptoms or pain, who are above the age of 85, and who most recently dialyzed via HD as opposed to PD.
Voluntary dialysis withdrawal raises key ethical dilemmas. If a patient chooses to withdraw from dialysis, how is a nephrologist legally and ethically obligated to respond? Along with other countries around the world, UK and US legislation align with the recommendations of the World Medical Association to allow an individual to refuse medical treatment. In the US, the passage of the Patient Self-Determination Act in 1990 required health agencies to provide patients with advance directives and information regarding the right to refuse therapy. However, it is critical for a patient’s decision-making capacity to first be established. An individual with capacity can comprehend a decision’s consequences, deliberate about choices, communicate wishes, and choose an option most concordant with personal values and beliefs. No formal practical guidelines exist for capacity determination, but structured interviews based on models such as the MacArthur Competency Assessment Tool may help.
The American Society of Nephrology’s (ASN’s) recommendations via the Choosing Wisely campaign has urged nephrologists to elicit goals, discuss prognosis, and evaluate risks and benefits before deciding to withhold or initiate dialysis. Building upon this, the RPA has developed guidelines (later endorsed by the ASN) suggesting that dialysis be withdrawn or withheld for the following patients:
- those with decision-making capacity who refuse dialysis
- those without decision-making capacity who have previously indicated a desire for refusal in an oral or written advance directive
- those without decision-making capacity whose legal surrogate refuses dialysis
- those with irreversible neurological impairment
- those whose medical condition precludes the technicalities of the dialytic procedure (eg, dementia, profound hemodynamic instability)
- those with Stage 5 CKD older than 75 who meet two of the following criteria
- nephrologist would not be surprised if the patient were to die within a year
- high comorbidity score (eg, modified Charlson Comorbidity Index score > 8 or high Elixhauser Comorbidity Index)
- impaired functional status (eg, Karnofsky Performance Scale Index score < 40)
- severe malnutrition (eg, serum albumin < 2.5 g/dL)
The RPA also advocates for using time-limited trials of dialysis for individuals with uncertain prognosis or for whom a consensus regarding dialysis withholding or withdrawal cannot be reached. Some experts point out that because decisions to start or stop treatment should always involve shared decision-making, distinctions between withholding and withdrawing dialysis may be morally irrelevant. Ultimately, the involvement of a multidisciplinary team consisting of nephrologists, nurses, palliative care subspecialists, chaplains, and lawyers may be needed to navigate these ethical dilemmas.
EOL care for seriously ill, hospitalized adults appears to be improving since the findings of the Study to Understand Prognoses and Preferences for Outcomes and Risks of Treatment (SUPPORT) investigators. However, patients on dialysis continue to have lower quality of EOL care compared to other patients with serious illnesses. In a retrospective analysis of 57,753 individuals who died in an inpatient facility within the Veterans Affairs health system between 2009 and 2012, patients with ESKD died nearly twice as frequently in the intensive care unit as compared to those with malignancy or dementia. Families of patients with ESKD also reported poorer quality of EOL care in comparison to families of individuals with other chronic illnesses.
Continuing to effectively address EOL needs will require training the future workforce for competency in this area, development of EOL quality metrics specific to kidney disease, measurement of the potential fiscal impact of achieving these metrics, and continued advocacy for culture change. These efforts are time-intensive but may be what is needed for nephrologists to protect and uphold nonmaleficence for their patients.
Dialysis for Patients at End-of-Life (Justice)
The increasing age and comorbid disease burden of patients with ESKD have made discussing non-dialytic, conservative management a requisite component of person-centered care. But what about situations in which patients who are terminally ill wish to continue dialysis and have access to resources such as hospice? The ethical principle of justice requires fairness in all medical decisions as well as an equal distribution of resources.

Copyright: Zolnierek / Shutterstock
If we fail to advocate for universal coverage of dialysis for all terminally ill patients with ESKD, are we at risk of sacrificing justice?
Palliative care, the provision of emotional, spiritual, and physical symptom-related support throughout a serious illness continuum is distinct from hospice care, which refers to the provision of these services to an individual who is terminally ill. Founded in the UK by Dame Cecily Saunders in 1967 and galvanized in the US five years later by Dr. Elisabeth Kubler-Ross, hospice services have made remarkable contributions to alleviating human suffering. In 1986, the Medicare Hospice Benefit was made permanent by the US Congress, and states were given the additional option of incorporating hospice services into their Medicaid programs. The use of hospice has steadily increased since then, and in 2017, approximately 1.5 million Medicare beneficiaries were enrolled in hospice care.
In order for an individual to be eligible for hospice under the US Medicare model, he or she must be deemed by two physicians to have a life expectancy of six months or less. Given the prognostic uncertainty associated with many chronic conditions, how is this determination made? CMS has provided both general and disease-specific guidelines to help physicians make this determination. General criteria include failure to thrive, cognitive decline, increasing functional dependence, and various end-organ manifestations of severe chronic illness. Disease-specific criteria for a patient with CKD to be deemed terminally ill include any of the following:
- creatinine clearance <10 cc/min, or <15 cc/min with comorbid congestive heart failure
- serum creatinine > 8 mg/dL
- other signs and symptoms of kidney failure, including uremia, oliguria, intractable hyperkalemia, uremic pericarditis, hepatorenal syndrome, and intractable fluid overload
Aside from the difficulties with using these specific criteria to precisely estimate the illness trajectory of a patient with CKD, other ethical dilemmas arise with regards to resource allocation for these patients. Though ESKD has officially been made a hospice-appropriate diagnosis, rates of hospice use among patients with ESKD remain low and lag behind those with malignancies, likely in part reflecting the reluctance of hospice providers to risk non-reimbursement for patients on dialysis. Currently, Medicare only provides hospice coverage for patients with a terminal illness unrelated to kidney disease. Patients for whom ESKD is the terminal illness must stop dialysis prior to receiving Medicare coverage for hospice. As the decision to withdraw from dialysis is a difficult one, this policy may cause unnecessary distress for patients with ESKD and their caregivers.
In addition to improving patient well-being, changing policies to facilitate timely hospice referral may also have economic benefits. Medicare spending under the hospice benefit was greater than $10 billion in the year 2007 and continues to rise. In an analysis of 770,191 patients with ESKD, roughly 42% of dialysis patients on hospice were enrolled in these services for three days or less prior to death, likely an insufficient time frame to provide sufficient psychosocial support to both patients and their families. Rates of intensive care utilization and associated Medicare costs were similar to those not enrolled in hospice.

Visual Abstract by @krithicism on Wachterman et al
Can existing policy and models of care delivery be altered to allow for Medicare coverage of time-limited trials of dialysis for terminally-ill ESKD patients?
Concerns exist regarding resource allocation and costs, but the RPA guidelines acknowledge that some patients with a non-kidney disease-related terminal illness may actually benefit from and choose to receive dialysis. Experts in this area have pointed to the need for Medicare to cover both hospice and dialysis benefits for elderly patients, negotiate with pharmaceutical companies to lower prices for medications used for symptom management, expand ESRD Seamless Care Organizations (ESCOs) to include non dialysis-dependent CKD, and incentivize home dialysis to reduce costs associated with hospitalization and transportation.
In Taiwan, national policies that pay for hospice care have decreased invasive procedures at the end of life, reduced medical costs, and increased overall hospice utilization for seriously ill patients with cancer. To uphold justice and strive for the equal distribution of resources among seriously ill patients with advanced kidney disease, advocating for changes to Medicare policy in the US may be the next step we need.
– Executive Team Member for this region: Timothy Yau, AJKD Social Media Editor. Follow him @Maximal_Change.
How to Claim CME and MOC
US-based physicians can earn 1.0 CME credit and 1.0 MOC point for reading this region.
- Register/log in to the NKF’s Professional Education Resource Center (PERC). If you select “Physician” in the drop-down menu during registration, the ABIM ID will pop up – make sure to complete this during registration to receive MOC points after course completion.
- Review the activity, disclosure, and accreditation information.
- Click “Continue” and review Course Instructions.
- Complete Post-Test. Please note: By selecting “Yes” to the participation questions for each region, the corresponding Post-Test questions will appear. Click “Save Draft” to save your responses and finish later. When you are ready to submit your answers, click “Preview” to review all responses, then click “Submit.”
- Click “Next” to complete the Evaluation form, then click“Submit.”
- Claim 1.0 CME credit and 1.0 MOC point per region (up to 8.0 total for 8 regions of NephMadness).
- Save/print your certificate.
The CME and MOC activity will expire on June 13th, 2020.


Leave a Reply