Highlights From the February 2022 Issue
Editor’s Note: We asked authors of Original Investigations to provide short plain-language summaries that would briefly summarize what inspired their study, the basic approach taken, what was learned, and why it matters. We hope our readers will find this valuable in helping them keep up with the latest research in the field of nephrology. From the February 2022 issue:
Association Between Deceased Donor Acute Kidney Injury Assessed Using Baseline Serum Creatinine Back-Estimation and Graft Survival: Results From the French National CRISTAL Registry by Rémi Lenain et al
From the authors: Although deceased-donor acute kidney injury (AKI) portends an increased risk of delayed graft function in the short term, its impact on long-term graft survival is a matter of ongoing debate. Most of the existing studies did not show any association between donor AKI and graft survival. By refining the donor AKI classification in accordance with international guidelines, we found that not only ongoing donor AKI but also the presence of at least one abnormal serum creatinine value during procurement were associated with lower graft survival in kidney transplant recipients.
DOI: 10.1053/j.ajkd.2021.06.022
Editorial: Underscoring the Case for Better Markers of Kidney Injury in Deceased Donors by Sumit Mohan and Chirag R. Parikh [FREE]
Economic Impact of Donating a Kidney on Living Donors: A Korean Cohort Study by Sehoon Park et al
From the authors: The economic impact on living donors from donating a kidney for transplantation is a relevant concern for individuals considering becoming a donor and for policy-makers hoping to promote kidney donation. This nationwide study in Korea compared living kidney donors with a matched comparison group and found that living kidney donors had an elevated risk of losing stable employment and experiencing worsened economic status. A limitation of this study is that selection bias and unmeasured confounding factors may have contributed to these findings. Because our study found that voluntary living kidney donors in South Korea had worsened economic outcomes than a matched com-parison group, the socioeconomic impact on these donors should be considered in conjunction with the potential long-term adverse health outcomes after donation.
DOI: 10.1053/j.ajkd.2021.07.009
Editorial: Understanding and Overcoming Financial Risks for Living Organ Donors by Krista L. Lentine et al [FREE]
SARS-CoV-2 Antibody Response After a Third Dose of the BNT162b2 Vaccine in Patients Receiving Maintenance Hemodialysis or Peritoneal Dialysis by Ilias Bensouna et al [FREE]
From the authors: Since April 2021, the French National Authority for Health has recommended systematic use of a third dose of COVID-19 vaccine for dialysis patients to boost immunity. This study assessed vaccine response after the second and third doses by measuring patients’ antibody levels. Although most of the patients produced anti-bodies after 2 vaccine doses, some of them (mainly elderly patients and those receiving treatments that suppress immunity) had relatively low antibody levels. After a third booster dose, almost all patients increased their antibody levels, especially when the third dose was delayed. A third dose was not associated with greater side effects than the second dose. The relationship between increased antibody levels after a third dose and protection against clinical illness with COVID-19 remains to be evaluated.
DOI: 10.1053/j.ajkd.2021.08.005
Editorial: SARS-CoV-2 Vaccine in Dialysis Patients: Time for a Boost? by Karen M. Krueger et al [FREE]
Lung Ultrasound to Diagnose Pulmonary Congestion Among Patients on Hemodialysis: Comparison of Full Versus Abbreviated Scanning Protocols by Nathaniel Reisinger et al
From the authors: Pulmonary congestion owing to fluid overload is common among patients with kidney failure on hemodialysis (HD) and contributes to excess morbidity and mortality in this population. Physical examination is an insensitive approach to detecting pulmonary congestion. Previous studies have shown that 28-zone lung ultrasound is a sensitive test for detecting the pulmonary congestion associated with adverse clinical outcomes. It is unknown whether abbreviated forms of lung ultrasound tests examining fewer than 28 zones have similar diagnostic sensitivity. In this comparative study, we found that several abbreviated lung ultra-sound protocols (4-, 6-, or 8-zone) performed similarly to 28-zone studies among patients with kidney failure on hemodialysis seeking care in an emergency department. We did not demonstrate mortality differences between those with no-to-mild and moderate-to-severe pulmonary congestion. These data suggest that abbreviated lung ultrasound may be useful for expeditious evaluation of pulmonary congestion.
DOI: 10.1053/j.ajkd.2021.04.007
Kidney Transplantation in Patients With Monoclonal Gammopathy of Renal Significance (MGRS)–Associated Lesions: A Case Series by Cihan Heybeli et al
From the authors: Data on kidney transplantations in patients with monoclonal gammopathy of renal significance (MGRS)–associated kidney disease are limited because of the risk of recurrence that had discouraged kidney transplantations in these patients. This case series re-ports a single center’s experience with and without treatment of MGRS before kidney transplantation. Recurrence was common in patients who did not receive treatment for MGRS before kidney trans-plantation. Histologic recurrence was often responsible for graft loss, and hematologic relapse/progression was frequently the cause of death. Achieving a complete response before kidney transplantation appeared to reduce the risk of recurrence/relapse and possibly improved overall survival. Treatment of the MGRS seemed to stabilize allograft function in many of those who experienced relapse, but allograft losses and deaths still occurred despite hematologic response. Outcomes of MGRS after kidney transplantation are heterogeneous, and more studies are needed to determine the optimal hematologic response before proceeding to kidney transplantation and to identify optimal treatment of recurrences.
DOI: 10.1053/j.ajkd.2021.04.015
A Predictive Model for Progression of CKD to Kidney Failure Based on Routine Laboratory Tests by Helena U. Zacharias et al
From the authors: A novel risk equation for the timely identification of chronic kidney disease (CKD) patients at risk for progressing to kidney failure requiring kidney replacement therapy was developed in 4,915 patients with CKD stages 1-5 with and without albuminuria from the German Chronic Kidney Disease (GCKD) Study. It includes 6 laboratory tests: serum creatinine, albumin, cystatin C, and urea, in addition to hemoglobin and the urinary albumin-creatinine ratio. It achieved high predictive performance and good calibration both in a resampling approach in the GCKD study and in 3 in-dependent validation cohorts that included a total of 3,063 patients with CKD. Implementation of this risk equation in clinical practice holds promise for enhanced patient care.
DOI: 10.1053/j.ajkd.2021.05.018
Plasma Kidney Injury Molecule 1 in CKD: Findings From the Boston Kidney Biopsy Cohort and CRIC Studies by Insa M. Schmidt et al
From the authors: Kidney tubular injury may lead to the development or progression of chronic kidney disease (CKD). Plasma KIM-1 is a sensitive marker of tubular injury, but its association with adverse clinical outcomes across a spectrum of kidney diseases is not known. In 2 prospective cohort studies of individuals with common and diverse forms of chronic kidney disease, higher plasma KIM-1 levels were independently associated with progression to kidney failure. In individuals who under-went a native kidney biopsy with adjudicated histopathology, higher plasma KIM-1 levels were associated with more severe acute tubular injury, tubulointerstitial inflammation, and mesangial expansion. Collectively, the findings suggest that measurement of plasma KIM-1 levels may serve as a noninvasive tool to assess histopathologic lesions and has prognostic value across a variety of kidney diseases.
DOI: 10.1053/j.ajkd.2021.05.013
Canagliflozin and Kidney-Related Adverse Events in Type 2 Diabetes and CKD: Findings From the Randomized CREDENCE Trial by Hiddo J. L. Heerspink et al
From the authors: Canagliflozin reduced the risk of kidney failure and slowed the progression of kidney disease in people with type 2 diabetes and chronic kidney disease in the CREDENCE trial. This analysis examined kidney-related safety in the overall trial population and in subgroups based on kidney function. Results show that canagliflozin is safe for the kidneys, with fewer kidney-related safety events, even among patients with more severe kidney disease at the start of the trial. Among patients in whom acute kidney injury developed during the trial, fewer in the canagliflozin group died or required dialysis compared with the placebo group. These data support the positive benefit/risk profile of canagliflozin in the high-risk population of people with type 2 diabetes and chronic kidney disease.
DOI: 10.1053/j.ajkd.2021.05.005
Prognostic Significance of Urinary Biomarkers in Patients Hospitalized With COVID-19 by Steven Menez et al [FREE]
From the authors: Acute kidney injury is a serious complication in patients hospitalized with coronavirus disease 2019 (COVID-19). We hypothesized that biomarkers measured in the urine that are more specific for kidney injury and inflammation than serum creatinine may add to our understanding of kidney injury in the setting of COVID-19. We found that certain biomarkers—including epidermal growth factor and kidney injury molecule 1, among others—were associated with severe acute kidney injury, dialysis, and death within 60 days in patients hospitalized with COVID-19. Our study results suggest that these studied biomarkers may help identify patients at particularly high risk for adverse kidney outcomes.
DOI: 10.1053/j.ajkd.2021.09.008
Special Report from the February 2022 Issue:
Atherosclerotic Renovascular Disease: A KDIGO (Kidney Disease: Improving Global Outcomes) Controversies Conference by Caitlin W. Hicks et al [OPEN ACCESS]
In February 2020, KDIGO (Kidney Disease: Improving Global Outcomes) convened a Controversies Conference on central and peripheral arterial diseases in chronic kidney disease (CKD) in Dublin, Ireland. The objectives were to examine the current state of knowledge about cerebrovascular diseases, central aortic disease, renovascular disease, and peripheral artery disease in persons with CKD and to determine what needs to be done in these areas to improve patient care and outcomes. An executive summary of the conference proceedings has been published elsewhere. The conference included a total of 10 international experts who specifically focused on the topic of atherosclerotic renovascular disease (ARVD), including nephrologists, cardiologists, interventional radiologists, and vascular surgeons. Here, those experts and the conference leadership provide a more detailed expert consensus summary of the epidemiology, pathophysiology, investigation, and management of ARVD, as well as research recommendations for future consideration.
DOI: 10.1053/j.ajkd.2021.06.025
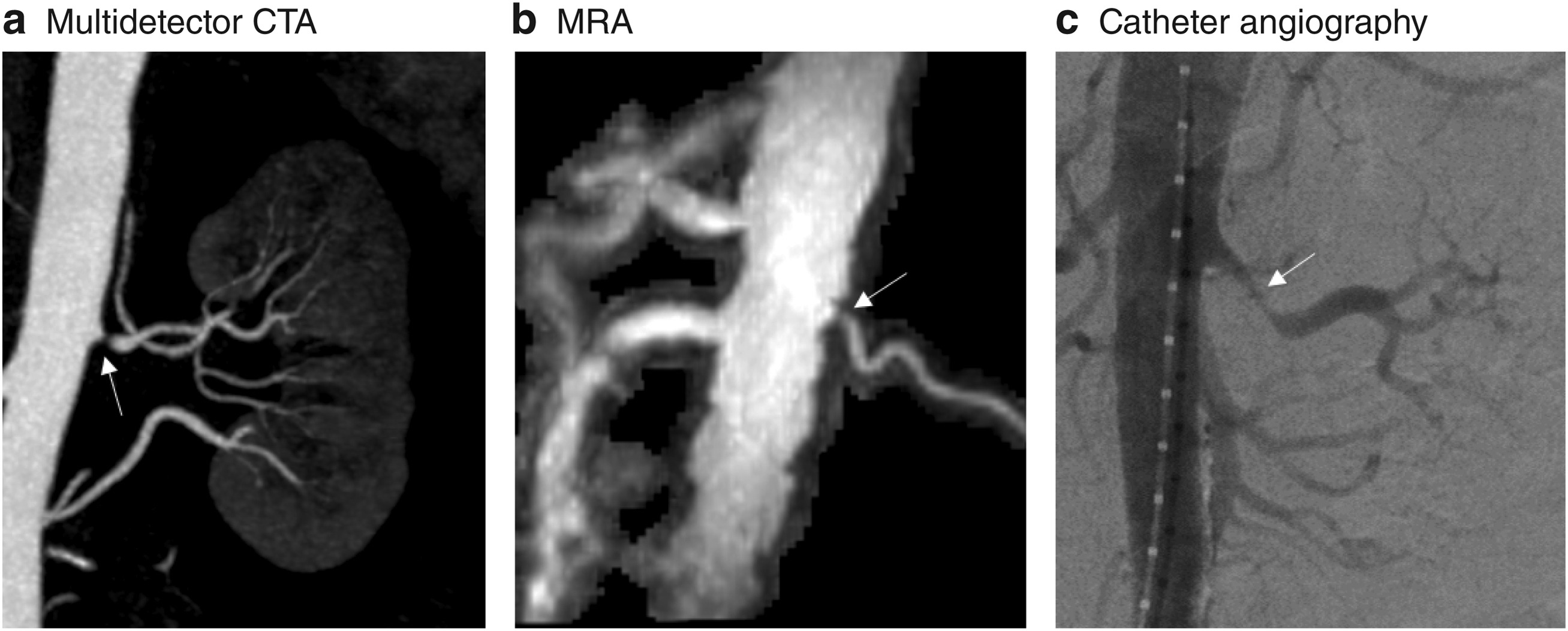
Figure 2 from Hicks et al, AJKD © The Authors
Blog Post Atherosclerotic Renovascular Disease: A Panel Discussion with Timothy Yau, Roger Rodby, William Whittier, and Pravir Baxi [FREE]
 On the Cover: In 1938, high above the brand new building 1 at the National Institutes of Health’s Bethesda campus, final touches are applied to the flagpole that will bear the standard signaling the nation’s deep commitment to enhancing health through biomedical research. Building 1 was the first of 6 buildings replacing the previous campus in central Washington, DC. When completed in June 1940, the Bethesda site tripled the NIH’s laboratory and administrative complex with its own power plant, ventilation systems, chemical hoods, animal rooms, sewage system, and power supply. The new campus contained dedicated space for research in industrial hygiene, public health, chemistry, pharmacology, zoology, infectious diseases, and cancer. Today, the NIH’s more than 75 buildings spanning over 300 acres support many of the programs discussed in the National Kidney Foundation’s Position Statement on research funding that appears in this issue.
On the Cover: In 1938, high above the brand new building 1 at the National Institutes of Health’s Bethesda campus, final touches are applied to the flagpole that will bear the standard signaling the nation’s deep commitment to enhancing health through biomedical research. Building 1 was the first of 6 buildings replacing the previous campus in central Washington, DC. When completed in June 1940, the Bethesda site tripled the NIH’s laboratory and administrative complex with its own power plant, ventilation systems, chemical hoods, animal rooms, sewage system, and power supply. The new campus contained dedicated space for research in industrial hygiene, public health, chemistry, pharmacology, zoology, infectious diseases, and cancer. Today, the NIH’s more than 75 buildings spanning over 300 acres support many of the programs discussed in the National Kidney Foundation’s Position Statement on research funding that appears in this issue.
This image from 70 Acres of Science: The NIH Moves to Bethesda, by Michele Lyons, curator of the National Institutes of Health DeWitt Stetten Jr., Museum of Medical Research is courtesy of the Office of NIH History, and is in the public domain.
In 2017, we established an annual celebration of articles that our editorial team designated as “Editors’ Choice” selections. The editors are delighted to recognize five articles that have been selected to receive the 2021 Editors’ Choice Award. These articles will be freely available at AJKD.org until February 15, 2022.









Leave a Reply