Highlights from the July 2022 Issue
Editor’s Note: We asked authors of Original Investigations to provide short plain-language summaries that would briefly summarize what inspired their study, the basic approach taken, what was learned, and why it matters. We hope our readers will find this valuable in helping them keep up with the latest research in the field of nephrology. From the July 2022 issue:
Racial and Ethnic Disparities in Kidney Replacement Therapies Among Adults With Kidney Failure: An Observational Study of Variation by Patient Age by Adam S. Wilk et al
From the authors: Research has shown wide racial and ethnic disparities in use of kidney transplant and home dialysis, yet how age interacts with these disparities is unknown. We compared use of kidney replacement therapies between racial and ethnic groups among patients with incident kidney failure within age groups using registry data for 830,402 US adults (age >21 years) during the period of 2011-2018. Absolute disparities in transplant and home dialysis (outcomes measured at 90 days after treatment initiation) were most pronounced among patients aged 22-44 years. After adjusting for numerous patient-level factors, the largest disparities were observed for trans-plant among adults aged 22-44 years. These findings suggest that the needs of younger adults should be emphasized in designing interventions to reduce dis-parities in access to preferred kidney replacement therapies.
DOI: 10.1053/j.ajkd.2021.09.012
Editorial: Unmasking Disparities in Kidney Replacement Therapy Among Young Patients—A Call to Action by Katherine M. Wang Mallika L. Mendu [FREE]
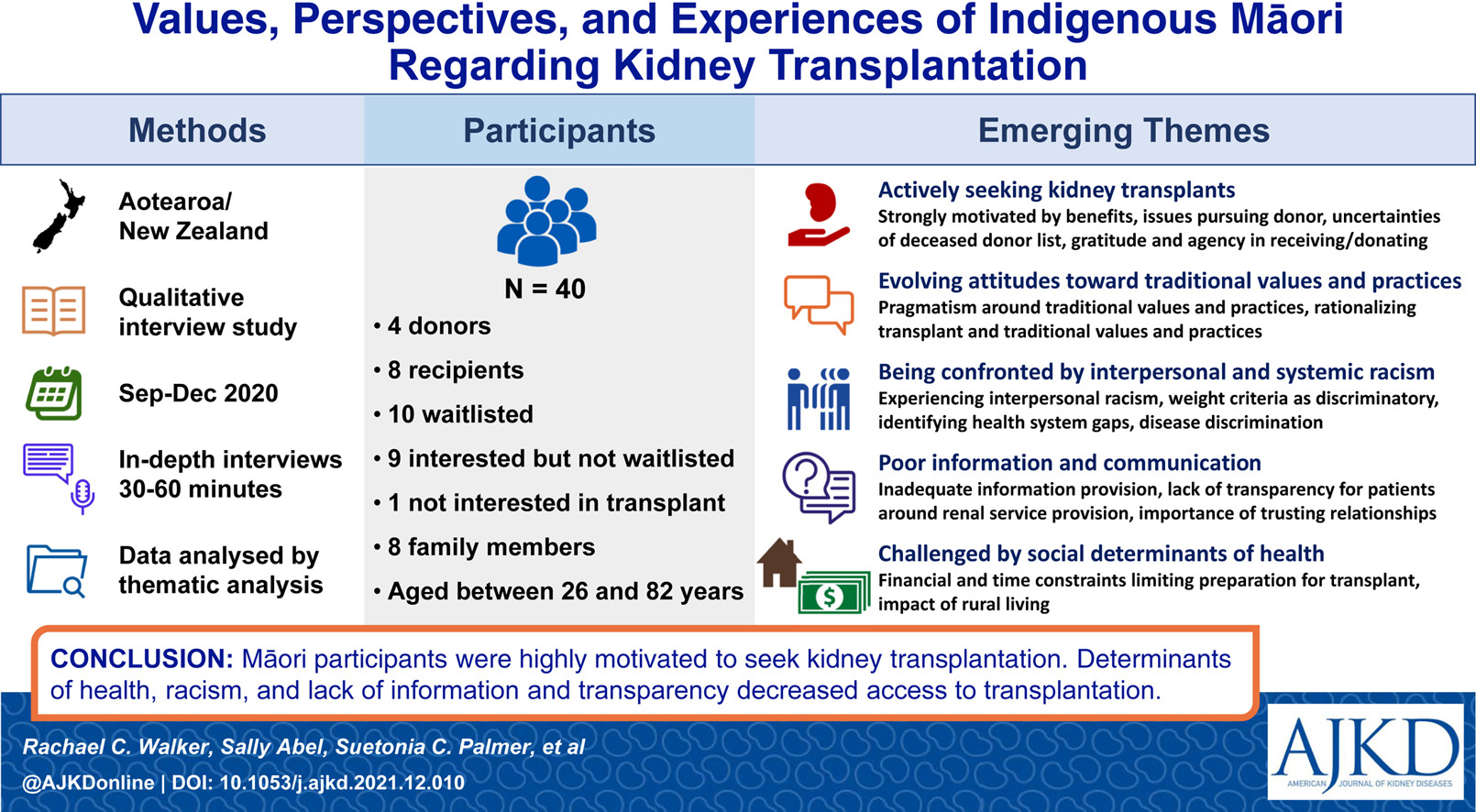
Values, Perspectives, and Experiences of Indigenous Māori Regarding Kidney Transplantation: A Qualitative Interview Study in Aotearoa/New Zealand by Rachael C. Walker et al
From the authors: Transplantation is the gold standard treatment for patients with advanced kidney disease; however, among Indigenous peoples transplantation incidence is much lower despite their substantially higher rates of advanced kidney disease. In this study, we interviewed Maori (Indigenous) patients with advanced kidney disease, kidney donors, and family members about their experiences with and views of kidney transplantation. The findings show that our participants are motivated to donate and receive a kidney transplant, but barriers to transplant delivery are described that may contribute directly to ongoing inequities.
DOI: 10.1053/j.ajkd.2021.12.010
Editorial: Breaking Down the Silence: Call for Action to Address Access Disparities to Transplantation in Indigenous Māori Peoples With Kidney Failure by Germaine Wong et al [FREE]
Patient Frailty and Functional Use of Hemodialysis Vascular Access: A Retrospective Study of the US Renal Data System by Karen Woo et al [OPEN ACCESS]
From the authors: We examined outcomes after arteriovenous fistula and graft placement in patients who initiated hemodialysis and were recorded in the US Renal Data System database from January 1, 2012, through October 31, 2015. Patients were categorized into quartiles of frailty, which is a state of increased vulnerability resulting from decreased physiologic function. Our findings demonstrated that patients who were the most frail had a significantly lower likelihood of successfully using a fistula compared with patients who were the least frail. Patients who were the most frail were also at the highest risk of mortality, suggesting that patients who are the most frail may not derive benefit from creation of an arteriovenous fistula.
DOI: 10.1053/j.ajkd.2021.10.011
Editorial: Tailoring Vascular Access for Dialysis: Can Frailty Assessment Improve the Fit? by Külli Kuningas Nicholas Inston [FREE]
Dialysis Nonadherence and Kidney Transplant Outcomes: A Retrospective Cohort Study by Deirdre Sawinski et al
From the authors: Transplant physicians use aspects of the dialysis prescription to judge adherence in transplant candidacy decisions, yet the link between these measures and posttransplant outcomes is unclear. Misapplication of these data has the potential to prevent dialysis patients from accessing transplants, and their exclusion on this basis may be unjustified. Using Cox proportional hazards and logistic regression modeling, we investigated the associations of hyperkalemia, hyperphosphatemia, large fluid gains, and shortened dialysis treatments with posttransplant outcomes. Our finding that high potassium and phosphorus levels are not consistently related to patient or allograft survival suggests that clinicians should not exclude transplant candidates on this basis.
DOI: 10.1053/j.ajkd.2021.09.011
Recovery From Dialysis-Treated Acute Kidney Injury in Patients With Cirrhosis: A Population-Based Study by Peter L. Wang et al
From the authors: Hospitalized patients with cirrhosis and kidney injury requiring dialysis are often critically ill and have high mortality rates. Our population-based retrospective observational study of these patients from 2009 to 2016 shows that one quarter of patients recover kidney function sufficiently to discontinue dialysis by 3 months, whereas the remaining patients have a high rate of death. Patients who were waitlisted for a liver transplant or admitted to a teaching hospital had higher rates of recovery, whereas those with higher Model for End-Stage Liver Disease scores and sepsis did worse. These results can inform patients, their families, and their care providers when making decisions on initiating dialysis and assessing prognosis.
DOI: 10.1053/j.ajkd.2021.09.025
Rates of Reversal of Volume Overload in Hospitalized Acute Heart Failure: Association With Long-term Kidney Function by Wendy McCallum et al
From the authors: For patients with heart failure, fluid accumulation in the lungs or other parts of the body causing shortness of breath or swelling usually prompts hospital admission. During the process of fluid removal, or decongestion, it is unknown whether the kidneys are placed at risk of worse longer term function if decongestion occurs at a faster rate. This study examined whether the rate of decongestion during hospitalizations for heart failure was associated with an increased risk of worse kidney function in the 10-month period after discharge, using 3,500 participants from the previously conducted EVEREST trial. The results show that more rapid decongestion did not increase the risk of worse longer term kidney function.
DOI: 10.1053/j.ajkd.2021.09.026

Fig 1 from McCallum et al, AJKD © National Kidney Foundation, showing the association between change in (A) markers of volume overload and (B) markers of hemoconcentration with risk of incident CKD G4-G5.
Blog Post Rapid Decongestion in Persons Hospitalized with Heart Failure by Carl Walther [FREE]
Association of GSTM1 Deletion With Progression of CKD in Children: Findings From the Chronic Kidney Disease in Children (CKiD) Study by Rebecca V. Levy et al
From the authors: Although chronic kidney disease is rare in children, it may cause significant harm when it occurs. In this study, we used a multicenter cohort of children with chronic kidney disease to test the association of GSTM1 deletion with progression of kidney disease. We found that children with nonfunctional GSTM1 alleles were almost twice as likely to lose half their kidney function or to need kidney replacement therapy as were children with 2 functioning alleles. Differences in GSTM1 status were not associated with cardiovascular outcomes or remission of proteinuria. This finding could help to identify children who could benefit from closer monitoring.
DOI: 10.1053/j.ajkd.2021.10.007
Plasma Lead Concentration and Risk of Late Kidney Allograft Failure: Findings From the TransplantLines Biobank and Cohort Studies by Camilo G. Sotomayor et al [OPEN ACCESS]
From the authors: Heavy metals are known to induce kidney damage, and transplanted kidneys may be particularly susceptible. Recent evidence showed that plasma concentrations of the heavy metals cadmium and arsenic are associated with increased risk of kidney graft failure. It is unknown if this association is also true for plasma lead concentrations. We measured plasma lead concentrations in 670 kidney transplant recipients with a functioning graft for ≥1 year who were followed for approximately 5 years at our outpatient clinic in Groningen, The Netherlands. Plasma lead concentrations were independently associated with an increased risk of late kidney graft failure, suggesting that lead-targeted interventions could be examined in future research as novel strategies to decrease the burden of kidney allograft failure.
DOI: 10.1053/j.ajkd.2021.10.009
Higher-Dose Gabapentinoids and the Risk of Adverse Events in Older Adults With CKD: A Population-Based Cohort Study by Flory T. Muanda et al
From the authors: Gabapentinoids, including gabapentin and pregabalin, are frequently prescribed as opioid alternatives. Given that gabapentinoids are eliminated from the body by the kidney, we sought to determine the risk of serious adverse events in patients with chronic kidney disease who started a gabapentinoid at a higher versus a lower dose. We conducted a population-based study to answer this question. For every 250 patients who star-ted gabapentin or pregabalin at a higher dose (>300 and >75 mg/d, respectively) versus a lower dose, 1 patient visited a hospital with encephalopathy, a fall, or a fracture or was hospitalized with respiratory depression. If verified, the risk of higher-dose gabapentinoids should be balanced against the benefit of using a higher dose.
DOI: 10.1053/j.ajkd.2021.11.007
Perspective from the July 2022 Issue:
A Participant-Centered Approach to Understanding Risks and Benefits of Participation in Research Informed by the Kidney Precision Medicine Project by Catherine R. Butler et al [OPEN ACCESS]
An understanding of the ethical underpinnings of human subjects research that involves some risk to participants without anticipated direct clinical benefit—such as the kidney biopsy procedure as part of the Kidney Precision Medicine Project (KPMP)—requires a critical examination of the risks as well as the diverse set of countervailing potential benefits to participants. This kind of deliberation has been foundational to the development and conduct of the KPMP. Herein, we use illustrative features of this research paradigm to develop a more comprehensive conceptualization of the types of benefits that may be important to research participants, including respecting pluralistic values, supporting the opportunity to act altruistically, and enhancing benefits to a participant’s community. This approach may serve as a model to help researchers, ethicists, and regulators to identify opportunities to better respect and support participants in future research that entails some risk to these participants as well as to improve the quality of research for people with kidney disease.
DOI: 10.1053/j.ajkd.2021.10.006
 On the Cover: This striking image provides beautiful contrasting textures of weathered paint that has been slowly chipped away by many years of exposure to the elements. Lead, a common additive to paint used in many homes built before 1960, creates health risks when paint chips are ingested, especially by children. Among other health consequences, heavy metals like lead have been demonstrated to induce kidney damage. In this month’s issue of AJKD, Sotomayor and colleagues examine the relationship of kidney allograft failure and plasma lead concentration. They demonstrate that elevated plasma lead concentrations are associated with kidney allograft failure.
On the Cover: This striking image provides beautiful contrasting textures of weathered paint that has been slowly chipped away by many years of exposure to the elements. Lead, a common additive to paint used in many homes built before 1960, creates health risks when paint chips are ingested, especially by children. Among other health consequences, heavy metals like lead have been demonstrated to induce kidney damage. In this month’s issue of AJKD, Sotomayor and colleagues examine the relationship of kidney allograft failure and plasma lead concentration. They demonstrate that elevated plasma lead concentrations are associated with kidney allograft failure.
The photograph “Texture A 5-8-12” is by David Gunter is released on Flickr under the CC BY 2.0 license
Special 40th Anniversary Collection: DIALYSIS
AJKD is celebrating its 40th year of publication. In this special collection, the editors highlight landmark papers on dialysis that have been published in the journal over the past four decades.




Leave a Reply