#NephMadness 2023: Transitions of Care Region
Submit your picks! | NephMadness 2023 | #NephMadness | #TransitionsRegion
Selection Committee Member: Rasheeda Hall @Rasheeda_HallMD
Rasheeda Hall is a physician-scientist in the Division of Nephrology at Duke University. Her research focuses on adapting geriatric models of care into kidney care settings. Dr. Hall’s geriatric nephrology clinic at the Durham Veterans Affairs Healthcare System uniquely emphasizes geriatric assessment and conservative kidney management.
Writer: Alissar El Chediak @alissar_chediak
Dr. Alissar El Chediak is a transplant nephrology fellow at Vanderbilt University Medical Center. She was born and raised in Lebanon where she attended medical school and completed her internal medicine residency at the American University of Beirut. After that, she moved to the United States to pursue her nephrology fellowship at Vanderbilt. Dr. El Chediak’s research interests include increasing organ access to minorities, ABO-incompatible kidney transplant, treatment of COVID in kidney transplant patients, and simultaneous kidney and pancreas transplant.
Competitors for the Transitions of Care Region
Team 1: Supportive Care for Kidney Failure versus Team 2: Pediatric to Adult Care

Copyright: FGC/Shutterstock
Patients with kidney disease can undergo a lot of transitions throughout their care, whether it’s from pediatric to adult care, from chronic kidney disease (CKD) to end-stage kidney disease (ESKD), or from ESKD to transplantation. As nephrologists, we are perhaps most well-versed in the transition from advanced kidney disease to dialysis. In this region, we wanted to focus on two other critical transition periods: 1) the transition from advanced kidney disease to kidney supportive care, and 2) the transition from pediatric to adult care for the patient with kidney disease.
Team 1: Supportive Care for Kidney Failure
Dialysis is the default treatment for patients with advanced kidney disease, and it is relatively uncommon for patients who develop uremic signs and symptoms NOT to be initiated on dialysis. At the same time, observational studies show that for patients with significant comorbidities including advanced age, dialysis does not offer a survival advantage.

Copyright: Brian A Jackson/Shutterstock
Kidney supportive care varies amongst different levels of kidney disease. There are two models of management to focus on: first, conservative care of a patient with advanced CKD (ie, not initiating dialysis), and second, palliative care in patients with ESKD (ie, dialysis withdrawal).
Conservative management is a treatment option for patients with ESKD that, through shared decision-making and patient-centered approach, emphasizes quality of life without pursuing dialysis or transplantation. The focus is on slowing the decline in kidney function, active symptom management, advance care planning, and the provision of palliative care (Figure 1). Moreover, the goal is alleviation of suffering through empathic communication and support for psychosocial distress, especially since patients with advanced kidney disease have heavy symptom burden (whether physical or psychological).

Figure 1. Domains of kidney supportive care (adapted from Figure 1 in Kidney Supportive Care. Core Curriculum 2020)
Conservative care for patients with advanced CKD is a form of supportive care for those who choose not to initiate dialysis or pursue kidney transplantation. An example can be found at the University of Rochester Medical Center, where authors described their practice with shared decision-making in the cases of 13 patients who had chosen conservative management. The aim of the study was to test the authors’ hypothesis that offering conservative management depends on the willingness of nephrologists to learn and use primary palliative care skills. The study was a retrospective chart review conducted by two reviewers who determined the status of advance care planning, hospice referral, and place of death. One of the important findings was the participants’ perceptions of conservative management and their reasons for choosing it. These included poor prognosis, a wish to maintain their quality of life, a desire for a dignified life closure, and the intention to protect family members from having to see them suffer based on their own memory of having witnessed a relative on dialysis previously. Advance care planning was completed in 100% of the cases. Symptoms were managed in collaboration with primary care physicians. In this group of patients, their decisions to choose conservative management were influenced by their values and by previous experience with dialysis, in addition to their comorbidities and limited prognoses.
For a better understanding of patients who choose conservative care, a qualitative study at the University of Washington was conducted to determine their perception of conservative care, as described in decision aids developed outside the United States (Figure 2).
Conclusions from that study include the following:
1) Aspects of conservative care that were appealing to participants included a whole-person, team-based, and structured approach to care that focused on symptom management, maintaining current lifestyle, and managing health setbacks.
2) Participants were more receptive to conservative care when this was framed as an active rather than passive treatment approach, and were receptive to statements of uncertainty about future course of illness and prognosis.
3) Participants believed decisions about conservative care and dialysis should address considerations about risks and benefits of treatment options, family and clinician perspectives, and patient’s goals, values, and preferences.
4) Participants did not see conservative care and dialysis as mutually exclusive. To reiterate, older US patients with advanced kidney disease and their family members had difficulty with the notion of conservative care and dialysis as mutually exclusive care models.
 Figure 2. Perceptions of conservative care among patients with advanced kidney disease
Figure 2. Perceptions of conservative care among patients with advanced kidney disease
As for the second management option for patients with ESKD, some might choose the palliative route, wherein they stop dialysis. The lack of understanding of palliative care and/or negative perceptions among patients, caregivers, and providers alike may function as a barrier to a palliative approach in patients with advanced kidney disease. Few dialysis patients report having had even limited discussions about their wishes. The lack of discussions is likely fueled by provider uncertainty about prognosis and decreased exposure. System barriers include time constraints on patient visits, complexities associated with care coordination, lack of a supportive institutional culture, and an absence of appropriate financial reimbursement for conservative management in comparison to dialysis. One component of avoiding end-of-life discussion is the fear of abandonment and death. Particularly, family members feel as if they’re contributing to their loved one’s death, which is not the case. This is often fueled by a culture of medicine that values extension of life over quality of life.
As previously mentioned, many dialysis patients with life expectancy of <1 year may desire a palliative approach, which focuses on aligning patient treatment with patient’s informed preferences and discontinuing dialysis. This is described as a transition from conventional disease-oriented focused treatment to “patient- and family-centered care that optimizes quality of life by anticipating, preventing and treating suffering” as defined by the Centers for Medicare and Medicaid. The Kidney Disease: Improving Global Outcomes (KDIGO) and Renal Physicians Association/American Society of Nephrology (RPA/ASN) outlined recommendations regarding withdrawing dialysis for patients who fit certain criteria (Figure 3).
 Figure 3. Shared decision-making in dialysis
Figure 3. Shared decision-making in dialysis
Even though the transition to palliative care in ESKD patients is more common nowadays, there are several barriers hindering that transition. Figure 4 outlines the decision-making process for choice-driven dialysis withdrawal. Numerous barriers currently exist in the process and can be further categorized according to personal preference, cultural and religious beliefs, ethico-legal concerns, and policymaking priorities.

Figure 4. Decision-making process for choice-driven dialysis withdrawal.
In addition to identifying which patients might benefit from dialysis withdrawal, KDIGO, and RPA/ASN have also outlined recommendations regarding the approach to dialysis withdrawal. First, decision-making capacity is determined. Among patients with decision-making capacity, a multidisciplinary approach is taken to clarify their understanding of withdrawal from dialysis and to verify their intent. In those patients who don’t have decision-making capacity, any previously completed advanced directive or description of well-known, strongly held beliefs or values that would be inconsistent with dialysis (as verified by the health care surrogate or proxy) should be identified to guide further decisions. A systematic approach to discussing prognosis, treatment options, and goals of care should be implemented.
In conclusion, kidney supportive care aims to prevent and relieve suffering and enhance the quality of life of ESKD patients. Patients with kidney diseases can elect not to pursue further kidney replacement therapies (conservative care) or to discontinue them (dialysis withdrawal). These patients will need discussions on prognosis and end-of-life to be able to make decisions and plan according to their personal values. Unfortunately, there are barriers to transitioning to kidney supportive care in patients with advanced CKD. An integrated multidisciplinary approach involving patients, caretakers, and other members of the healthcare team is recommended.
Check out this podcast episode of The Cribsiders featuring AC Gomez:
#80 CKD and Transitions of Care
COMMENTARY BY JANE SCHELL:
Supportive Care for Kidney Failure for the Win
Team 2: Pediatric to Adult Care
The transition from pediatric to adult renal care is an intricate process requiring a multidisciplinary approach and thorough planning. The position paper from the Society for Adolescent Medicine in 1993 defined transition “as a process that involves purposeful, planned efforts to prepare the pediatric patient to move from caregiver-directed care to disease self-management in the adult unit.” This transition of care most often occurs in patients between 18 and 24 years of age, a critical time in the lives of young adults, when they experience unique challenges and when there is a substantial risk for nonadherence and poor outcomes.

Copyright: Darkdiamond67/Shutterstock
To young patients, an effective transition is important because it reinforces patient independence during early adult care visits. As for healthcare systems, high morbidity, and mortality are observed in unprepared patients after they transition their care to adult nephrologists, as demonstrated by a Canadian study of kidney transplant recipients (Figure 5).
 Figure 5. Usefulness and cost-effectiveness of a kidney transplant transition clinic
Figure 5. Usefulness and cost-effectiveness of a kidney transplant transition clinic
Several barriers exist to a successful transition toward adult care. Adult nephrologists often feel ill-equipped to facilitate a successful transition and most centers do not have protocols in place. As per the 2020 US Renal Data System (USRDS),<5% of patients with kidney failure in the United States are children or young adults. Adult providers face difficulties when dealing with adolescent patients who have chronic illness in addition to all of the other physical, psychological, and sexual changes in their development. All of that can make the management and transition difficult for the patient, families, and staff. As for the pediatric patients, they face their own set of challenges. These include difficulty navigating adult healthcare systems, gaps in insurance coverage, lack of health self-efficacy, and limited experience in self-management. After the transition to adult care, patients might feel isolated and disconnected from their new community of patients, providers, and other participants in the healthcare system. This can have a profound psychological impact on young patients with chronic kidney disease or kidney failure who are at high risk of depression, low self-esteem, and high-risk behavior.
The councils of both the International Society of Nephrology (ISN) and the International Pediatric Nephrology Association (IPNA) published a consensus statement describing the transition from pediatric to adult renal services, “Transfer should occur from pediatric to adult nephrology services only after efforts to assess and prepare the adolescent/young adult have occurred.” In short, not only should the physical aspects of the illness be addressed in the young patient, but also the impact upon educational, social, and psychological functioning. Only after all these issues have been tackled and the milestones of adolescence completed is it appropriate to transfer to the adult unit. This transfer should be individualized, taking into consideration psychological, educational, and financial factors. Collaboration between the patient, parents/caregivers, and physicians from both the adult and pediatric clinics must be attained. Transition of care should be gradual. As per the consensus statement, a transition clinic is recommended as an ideal method to endorse a successful transfer of care. Also, they suggested a Transition Scale as a tool to assess and monitor the attainment of goals of transition. Components of the Transition Scale include type of illness, treatment, adherence, nutrition, self-management skills, informed reproductive health, trade/school, insurance, ongoing support, and new health care providers.
Another published simplified approach to facilitate the transition from pediatric to adult renal care is the PREP approach (Figure 6).

Figure 6. PREP approach for pediatric to adult kidney care transition
Some centers have established transition programs and clinics. Northwestern Medicine Nephrology implemented a pilot transition-of-care program for young adults with kidney disease. This program provided coordination of care between pediatric and adult nephrology teams through a formal transition process. After 18 months, they evaluated the patients’ perception of the program and published their experience.
The authors also defined a successful transition as when a patient returned for follow-up at Northwestern Medicine at least once after the initial transfer visit. 71% of patients successfully transitioned to adult care, which is significantly higher than that reported in the literature. Patients were also asked to take an established survey to evaluate their perception of this process and assess their readiness for the transition. 82% of the participants that filled the questionnaire felt ready to transfer to adult care and 88% felt having a transition appointment and meeting the adult care providers in the pediatric setting to be valuable (Figure 7).
 Figure 7. A nephrology pediatric to adult transition clinic pilot program
Figure 7. A nephrology pediatric to adult transition clinic pilot program
Another example of a transition program was that of the dialysis and kidney transplant program at Children’s Mercy Hospital. They created the K.E.Y.S (Kidney Education for Your Success) program, which consists of four phases (Figure 8).
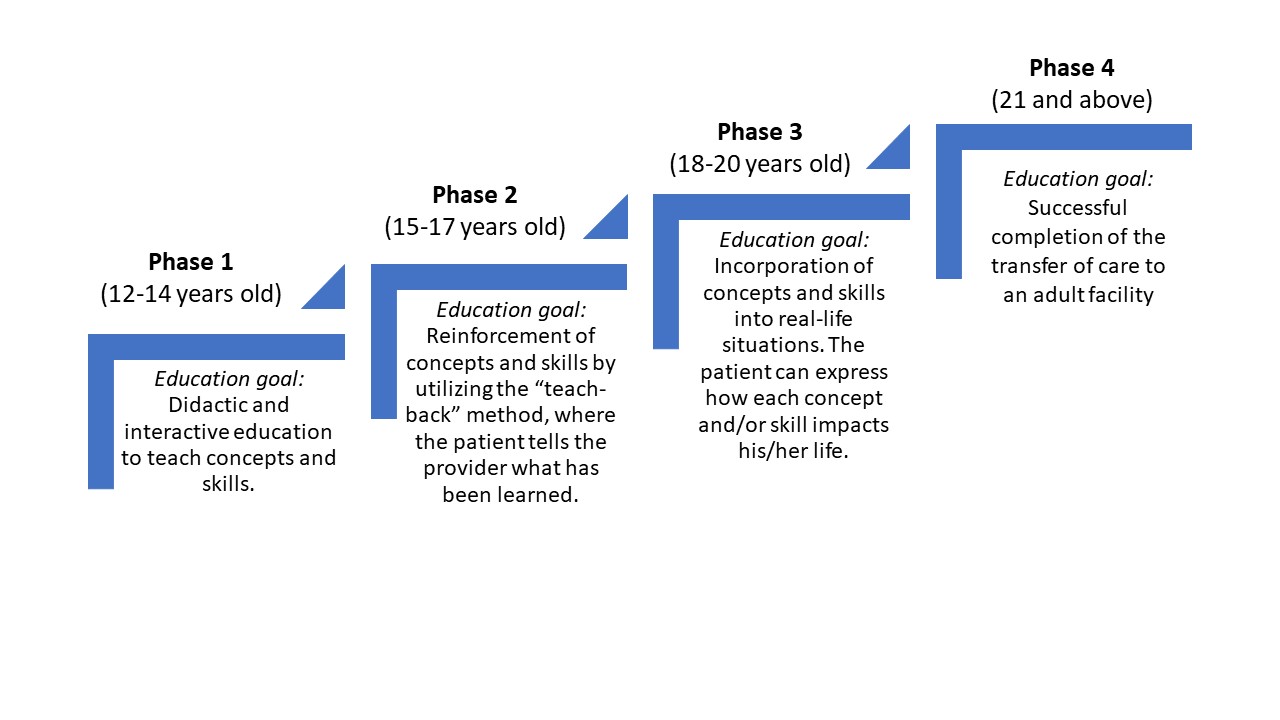
Figure 8. The K.E.Y.S program
Transitioning is a longitudinal process beginning in childhood and continuing through early adulthood. Barriers to this transition include delays in psychosocial milestones, academic challenges, and lack of collaboration between adult and pediatric teams in addition to the normal age-related vulnerability of the young adult years. Extra support in adult care for this vulnerable group is essential to help them successfully navigate their journey and can be accomplished using transition clinics. Building an effective transition program is not done overnight; it begins with small steps that progressively lead toward the defined goal with repeated cycles of assessment, analysis, and improvement.
– Executive Team Members for this region: Pascale Khairallah @Khairallah_P and Anna Vinnikova @KidneyWars
How to Claim CME and MOC
US-based physicians can earn 1.0 CME credit and 1.0 MOC per region through NKF PERC (detailed instructions here). The CME and MOC activity will expire on June 1, 2023.
Submit your picks! | #NephMadness | @NephMadness | #TransitionsRegion


Leave a Reply