Highlights from the May 2025 Issue
Editor’s Note: We asked authors of Original Investigations to provide short plain-language summaries that would briefly summarize what inspired their study, the basic approach taken, what was learned, and why it matters. We hope our readers will find this valuable in helping them keep up with the latest research in the field of nephrology.
Highlights from the May 2025 issue:
Patient and Health Care Provider Perspectives on Showering for Patients With Hemodialysis Central Venous Catheters: A Survey Study by Jhonna Collins et al. [OPEN ACCESS]
Patients receiving hemodialysis with a central venous catheter (CVC) as their dialysis access are often told not to shower. We surveyed dialysis health care providers and patients to better understand practices and preferences with regards to personal hygiene and CVC-related care. We found that many patients would like to shower and not being able to shower negatively impacts their daily lives. We also found that health care providers would like to allow patients to shower but are worried about infection risk. Patients are also worried about infection risk. Recommendations made to patients on showering were varied. The ability to safely shower is important to patients. Further study of the risks and benefits of showering among patients receiving hemodialysis through a CVC is needed.
DOI: 10.1053/j.ajkd.2024.11.006
EDITORIAL: To Shower or Not to Shower? Personal Hygiene, Safety, and Patient Choice in Hemodialysis Catheter Care by Shane A. Bobart and Tariq Shafi [FREE]
Kidney and Cardiovascular Outcomes Among Patients With CKD Receiving GLP-1 Receptor Agonists: A Systematic Review and Meta-Analysis of Randomized Trials by Jui-Yi Chen et al. [OPEN ACCESS]
From the authors: Glucagon-like peptide 1 (GLP-1) receptor agonists reduce body weight and improve glycemic control. They also have been shown to protect the heart and kidney in people with diabetes. However, the extrapolation of these findings to those with chronic kidney disease (CKD) is uncertain. This study meta-analyzed data from clinical trials focusing on patients with CKD and noted that GLP-1 receptor agonists may slow kidney disease progression and lower the risk of heart disease, stroke, and death. These findings suggest that GLP-1 receptor agonists offer multiple kidney and cardiovascular benefits to people with CKD.
DOI: 10.1053/j.ajkd.2024.11.013
EDITORIAL: GLP-1 Receptor Agonists for CKD: Remaining Issues or Mission Complete? by Vanja Kosjerina and Peter Rossing [FREE]
Uromodulin and Risk of Upper Urinary Tract Infections: A Mendelian Randomization Study by Kristin Vardheim Liyanarachi et al. [OPEN ACCESS]
Traditional studies have suggested that uromodulin, a protein produced by the kidneys, may reduce the risk of urinary tract infections (UTIs). The certainty of these findings is limited by the potential influence of unmeasured confounding factors. Therefore, we decided to address this concern by using genetic data to perform a two-sample Mendelian randomization analysis, a technique known to limit the influence of such factors. Our findings support the hypothesis that uromodulin in urine may have a protective role against upper UTIs. The findings were consistent across sensitivity and sex-specific analyses. Further research into the implications of these findings for the treatment of UTIs as well as the possible utility of urinary uromodulin as a diagnostic marker is warranted.
DOI: 10.1053/j.ajkd.2024.11.007
EDITORIAL: Uromodulin: Is There a Causal Relationship With Urinary Tract Infection Risk? by Azuma Nanamatsu
and Kaice A. LaFavers [FREE]
Prevalence of Severe Mental Illness and Its Associations With Health Outcomes in Patients With CKD: A Swedish Nationwide Study by Nanbo Zhu et al. [OPEN ACCESS]
From the authors: Patients with chronic kidney disease (CKD) frequently experience mental health problems, yet the prevalence and impact of severe mental illness (SMI) in this population remain uncertain. This Swedish nationwide study revealed that the prevalence of any SMI was 7.3% among patients with CKD (0.5% for schizophrenia, 2.1% for bipolar disorder, and 5.6% for major depressive disorder), representing a 56% higher prevalence than experienced by the Swedish general population. All 3 SMIs were associated with a higher mortality rate in patients with CKD, and bipolar disorder was also associated with a faster eGFR decline. Moreover, patients with CKD and schizophrenia or bipolar disorder exhibited a lower rate of initiating kidney replacement therapy. These findings highlight the need for improved recognition and management of SMI among people with kidney disease.
DOI: 10.1053/j.ajkd.2024.12.004
EDITORIAL: Severe Mental Illness in CKD: Why it Matters by S. Susan Hedayati [FREE]
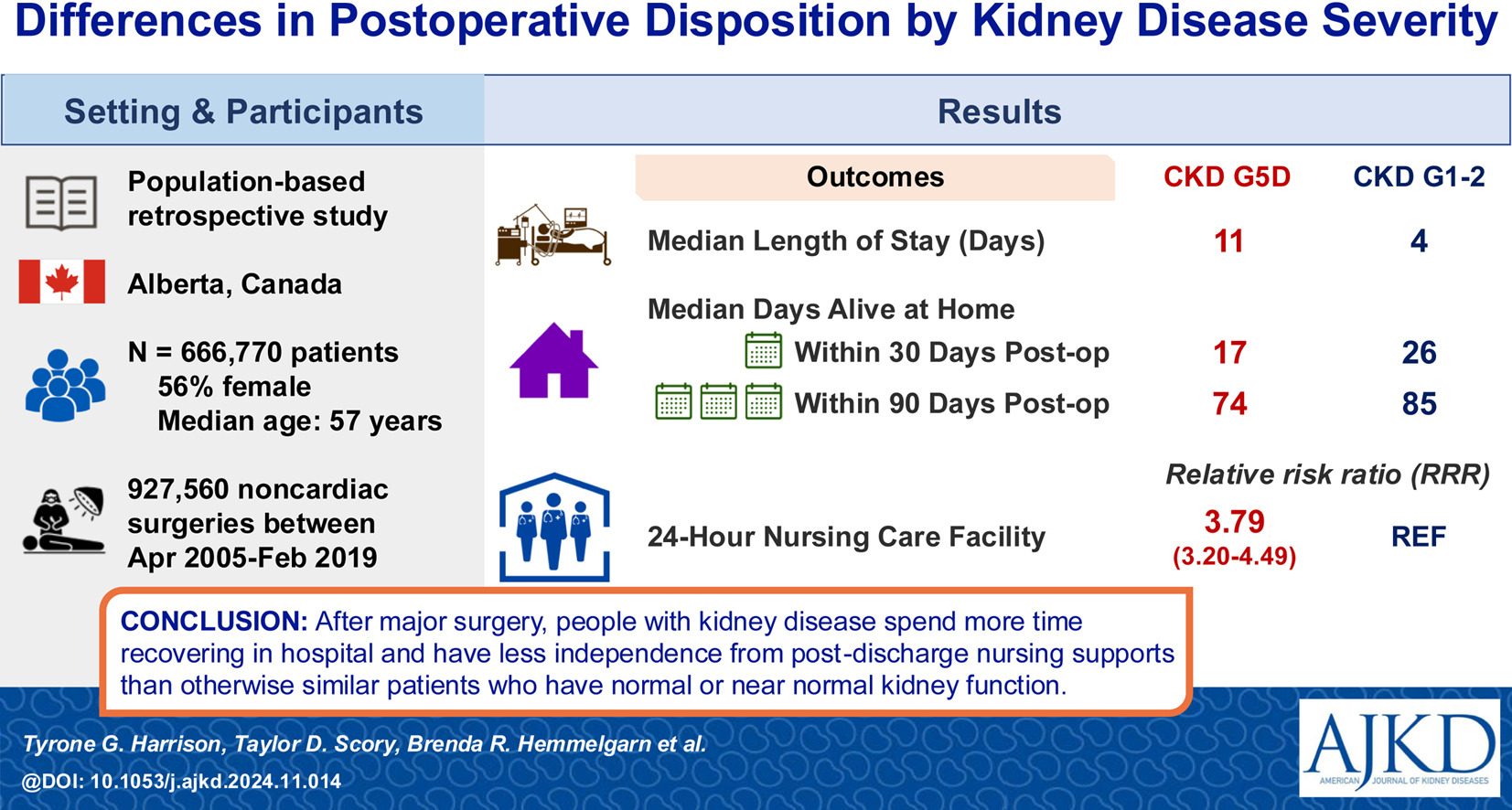
Differences in Postoperative Disposition by Kidney Disease Severity: A Population-Based Cohort Study by Tyrone G. Harrison et al. [OPEN ACCESS]
People with kidney disease have surgery more frequently, with worse outcomes, compared with others in the general population. However, little is known about how long they spend in hospital afterward and whether they will be discharged home or to other facilities. To understand this more, we examined nearly 1 million surgeries performed in Alberta, Canada. Compared with people who have normal kidney function and are undergoing surgery, people with the most advanced kidney disease spent more than 2 times longer in hospital and were more likely to be discharged to long-term care facilities instead of being discharged to their homes. Future research is needed to understand the factors that predict who will experience prolonged hospitalization and to develop interventions to enable earlier discharge for people with kidney disease.
DOI: 10.1053/j.ajkd.2024.11.014
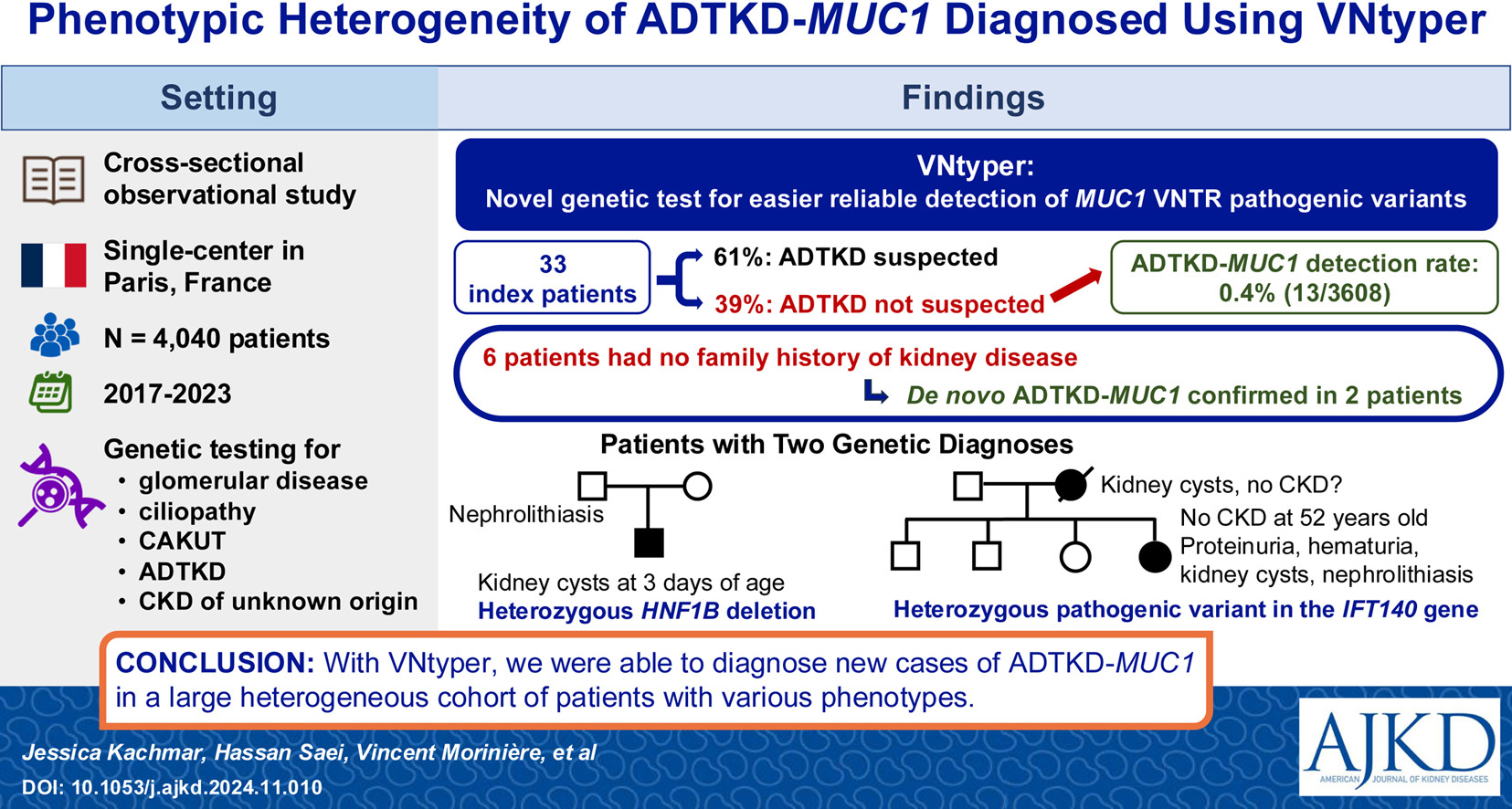
Phenotypic Heterogeneity of ADTKD-MUC1 Diagnosed Using VNtyper, a Novel Genetic Technique by Jessica Kachmar et al.
From the authors: Molecular diagnosis of autosomal dominant tubulointerstitial kidney disease due to variants in the MUC1 gene (ADTKD-MUC1) has long been challenging. Recently, we developed a computational pipeline named VNtyper to allow easier, reliable detection of MUC1 variants. When applied to a large heterogenous cohort of patients, it allowed us to diagnose ADTKD in patients in whom it had not been suspected. In some cases, this was due to 2 concomitant genetic diagnoses, which affected the phenotype. In others, there was no family history of kidney disease suggestive of an autosomal dominant disorder, and we were able to confirm de novo ADTKD-MUC1 in 2 patients.
DOI: 10.1053/j.ajkd.2024.11.010
Core Curriculum in Nephrology in the May 2025 issue:
Disorders of Volume: Core Curriculum 2025 by Nayan Arora and Sarah F. Sanghavi
In this Core Curriculum, the authors review the physiology of volume disorders and management strategies through a series of clinical cases. Historically, the paradigm for all maladies was associated with an imbalance of the 4 humors: blood, black bile, yellow bile, and phlegm. Although our understanding of disease has evolved significantly since the time of Hippocrates, a similar cornerstone of inpatient and ambulatory care involves understanding and correcting imbalances of volume. The kidneys are the principal organs controlling extracellular volume, capable of both sensing and altering salt retention through multiple redundant pathways, including the sympathetic nervous system and the renin-angiotensin-aldosterone system. Various disease states including sepsis, heart failure, and liver cirrhosis can dramatically alter the movement of volume across body compartments, leading to pathologic responses. Greater understanding of the role of the endothelial glycocalyx, the harms of volume overload among critically ill patients, and the impact of venous congestion on kidney function has challenged the traditional paradigms of volume management. Because both hypovolemia and hypervolemia are symptomatic conditions associated with adverse outcomes, managing volume is an essential skill for the nephrologist.
DOI: 10.1053/j.ajkd.2024.09.008
The maypole dance is a vibrant tradition of weaving ribbons around a central pole that symbolizes unity, connection, and shared joy within a community. Dancers move in harmony, each contributing to a collective pattern, much like each member of the interdisciplinary dialysis team plays a role in evaluating and strengthening the social connectedness of individuals with end-stage kidney disease (ESKD). In this issue of AJKD, Washington et al explain how fostering social bonds is crucial for the well-being of patients with ESKD. The authors present a theoretical framework for social connectedness and five recommendations to mitigate social disconnectedness.
Special thanks to Editorial Intern Benjamin Catanese for curating the cover image and drafting the cover blurb for this issue. The photograph “Maypole at Archer School for Girls (former Eastern Star Home) in Brentwood, Los Angeles, California” by Jennifer Arrow is released on Flickr under the CC BY-SA 2.0 deed license
SPECIAL ANNOUNCEMENT:
The NKF is actively seeking applications for an Editor-in-Chief to manage and lead the American Journal of Kidney Diseases (AJKD) for a 5-year term beginning January 1, 2027. Letters of Intent and a CV must be submitted by July 15, 2025. Please review the Call for Applications for complete details.







Leave a Reply