Highlights from the April 2021 Issue
Editor’s Note: We asked authors of Original Investigations to provide short plain-language summaries that would briefly summarize what inspired their study, the basic approach taken, what was learned, and why it matters. We hope our readers will find this valuable in helping them keep up with the latest research in the field of nephrology. From the April 2021 issue:
Effect of Intensive Urate Lowering With Combined Verinurad and Febuxostat on Albuminuria in Patients With Type 2 Diabetes: A Randomized Trial by Austin G. Stack et al [Open Access]
From the authors: People with chronic kidney disease and type 2 diabetes are at risk for deteriorating kidney function and progressive chronic kidney disease. Loss of albumin into the urine is an early marker of kidney damage and is associated with further deterioration. In this study, the combination of verinurad and febuxostat, drugs that reduce uric acid levels using different mechanisms, led to greater reductions in the amount of albumin in the urine and uric acid in the blood than did placebo. The treatment was generally well tolerated, with nausea and dizziness the most common adverse events seen after verinurad and febuxostat treatment. Although verinurad and febuxostat may help protect the kidneys against further decline in people with chronic kidney disease and type 2 diabetes, definitive assessment of their impact on preservation of kidney function awaits larger clinical studies.
DOI: 10.1053/j.ajkd.2020.09.009
Editorial: Urate Lowering With Combination Therapy in CKD: Reason for Optimism or Einstein’s Definition of Insanity? by Diana I. Jalal Glenn M. Chertow [FREE]
The Association of COVID-19 With Acute Kidney Injury Independent of Severity of Illness: A Multicenter Cohort Study by Dennis G. Moledina et al [FREE]
From the authors: One third of patients hospitalized with coronavirus disease 2019 (COVID-19) experience acute kidney injury (AKI), which is more than in other hospitalized patients. Patients with COVID-19 carry many well known risk factors for AKI, including severe lung disease requiring mechanical ventilation, shock, and significant inflammation. Whether higher rates of AKI in COVID-19 are greater than what could be expected in patients with similar risk factors is unknown. We compared AKI rates between those with and without COVID-19 after controlling for risk factors for AKI before and during hospitalization. We found that COVID-19 was independently associated with high rates of AKI. This indicates that some of the AKI risk in patients with COVID-19 is unexplained by traditional AKI risk factors and is unique to this disease.
DOI: 10.1053/j.ajkd.2020.12.007

Inpatient Pediatric CKD Health Care Utilization and Mortality in the United States by Zubin J. Modi et al
From the authors: Children with chronic kidney disease (CKD) often require hospitalization for various reasons. However, outcomes of this high-risk population are unknown. We used data collected from US hospitals to study the potential impact of CKD on hospitalization-related outcomes. We found that children with CKD had longer hospital stays, incurred higher health care expenses, and were at higher risk for death than children hospitalized for other chronic illnesses. Our study suggests that these associations are related to the higher degree of medical complexity among children hospitalized with CKD. Further investigation is needed to better understand the health care needs and delivery of care to hospitalized children with CKD.
DOI: 10.1053/j.ajkd.2020.07.024
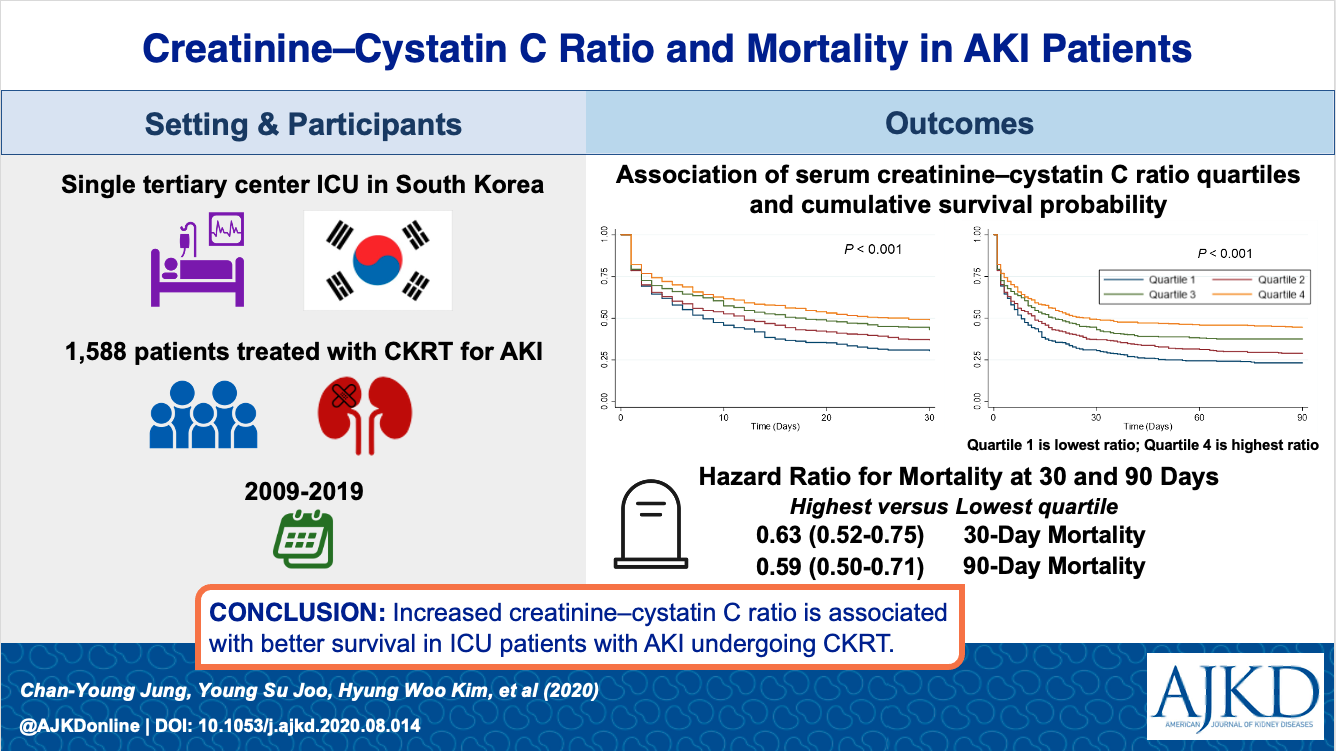
Creatinine–Cystatin C Ratio and Mortality in Patients Receiving Intensive Care and Continuous Kidney Replacement Therapy: A Retrospective Cohort Study by Chan-Young Jung et al
From the authors: Identifying risk factors for mortality in patients with acute kidney injury (AKI) receiving intensive care and continuous kidney replacement therapy (CKRT) is useful for improving the assessment of prognosis. In this study of 1,588 patients who underwent CKRT in a single tertiary center intensive care unit, 30- and 90-day mortality risks were significantly lower in patients with higher creatinine–cystatin C ratios at the time CKRT was begun. This association remained after adjustment for confounding factors. These findings suggest that creatinine–cystatin C ratio may be a simple, useful tool for mortality risk assessment in critically ill patients who develop AKI.
DOI: 10.1053/j.ajkd.2020.08.014
Also from the April 2021 Issue:
Qualitative Research in CKD: How to Appraise and Interpret the Evidence by Amanda Baumgart et al
From the authors: The value of patient-centered care, research, and policy is now widely recognized. This approach requires an in-depth understanding of the beliefs, values, and experiences of patients with chronic kidney disease (CKD) and their families, which may not always be conveyed in clinical settings. Qualitative research can generate detailed evidence on people’s priorities, goals, and needs to change practice and policy. Increasing understanding of the approaches used to evaluate and interpret qualitative studies may support efforts to translate findings to improve patient care and outcomes. We aim to provide a summary of qualitative research methods and guidance on appraising, interpreting, and applying qualitative studies.
DOI: 10.1053/j.ajkd.2020.12.011
 On the Cover: On this month’s cover, AJKD celebrates the 9th annual NephMadness, an educational initiative in which nephrology concepts vie in bracket matchups reminiscent of the US college basketball tournament. Contestants from around the world join in friendly competition to predict which “team” will be the most likely to change nephrology care in the next 5 years. Participants in the United States can claim up to 8.0 CME credits and MOC points.
On the Cover: On this month’s cover, AJKD celebrates the 9th annual NephMadness, an educational initiative in which nephrology concepts vie in bracket matchups reminiscent of the US college basketball tournament. Contestants from around the world join in friendly competition to predict which “team” will be the most likely to change nephrology care in the next 5 years. Participants in the United States can claim up to 8.0 CME credits and MOC points.
More information available at www.AJKDBlog.org
SPECIAL COLLECTION: WORLD KIDNEY DAY

In celebration of World Kidney Day on March 11, AJKD presents this special collection of recent publications from around the world addressing a variety of important aspects of kidney disease research. All articles are freely available until May 17, 2021.

Leave a Reply