Highlights from the January 2023 Issue
Editor’s Note: We asked authors of Original Investigations to provide short plain-language summaries that would briefly summarize what inspired their study, the basic approach taken, what was learned, and why it matters. We hope our readers will find this valuable in helping them keep up with the latest research in the field of nephrology. From the January 2023 issue:
Dipping Status, Ambulatory Blood Pressure Control, Cardiovascular Disease, and Kidney Disease Progression: A Multicenter Cohort Study of CKD by Silvio Borrelli et al [OPEN ACCESS]
From the authors: Among patients with chronic kidney disease (CKD), ambulatory blood pressure (BP) monitoring improves the identification of individuals at high risk of clinical disease outcomes. Those with uncontrolled ambulatory BP are known to have a higher risk of developing cardiovascular disease and kidney disease progression, particularly when their ambulatory BP does not decline by at least 10% at night. Whether this is also true for patients with presence of optimal ambulatory BP levels but a BP pattern of no nighttime decline is largely unknown. We measured ambulatory BP in 900 Italian patients with CKD and followed them for several years. We found that, independent of ambulatory BP level, the absence of nighttime reductions in BP was associated with worsening of CKD and more frequent cardiovascular events. The absence of nighttime declines in BP is an independent risk factor for adverse events among patients with CKD. Future studies are needed to examine whether treating the absence of nighttime declines in BP improves clinical outcomes.
DOI: 10.1053/j.ajkd.2022.04.010
Editorial: Clinical Value of Ambulatory Blood Pressure Monitoring in CKD by Alexander G. Logan [FREE]
Vaccine Attitudes and COVID-19 Vaccine Intention Among Parents of Children With Kidney Disease or Primary Hypertension by Chia-shi Wang et al
From the authors: Children with kidney disease or hypertension may do worse with COVID-19. As there are now effective vaccines to protect children from COVID-19, we wanted to find out what parents think about COVID-19 vaccines and what influences their attitudes. We surveyed and then interviewed parents of children who had received a kidney transplant, were receiving maintenance dialysis, had chronic kidney disease, or had hypertension. We found that two-thirds of parents were hesitant to vaccinate their children. Their reasons varied, but the key issues included the need for information pertinent to their child and a consistent message from doctors and other health care providers. These findings may inform an effective vaccine campaign to protect children with kidney disease and hypertension.
DOI: 10.1053/j.ajkd.2022.04.011
Editorial: Pediatric Vaccine Hesitancy and COVID-19 by Heather A. Morgans et al [FREE]
Prediction of Mortality and Major Adverse Kidney Events in Critically Ill Patients With Acute Kidney Injury by Javier A. Neyra et al
From the authors: Acute kidney injury (AKI) occurs commonly in critically ill patients admitted to the intensive care unit (ICU) and is associated with high morbidity and mortality rates. Prediction of mortality and recovery after an episode of AKI may assist bedside decision-making. In this report, we describe the development and validation of a clinical model using data from the first 3 days of an ICU stay to predict hospital mortality and major adverse kidney events occurring as long as 120 days after hospital discharge among critically ill adult patients who experienced AKI within the first 3 days of an ICU stay. The proposed clinical models exhibited good performance for outcome prediction and, if further validated, could enable risk stratification for timely interventions that promote kidney recovery.
DOI: 10.1053/j.ajkd.2022.06.004
Patient and Clinician Perspectives on Shared Decision Making in Vascular Access Selection: A Qualitative Study by Meghan J. Elliott et al
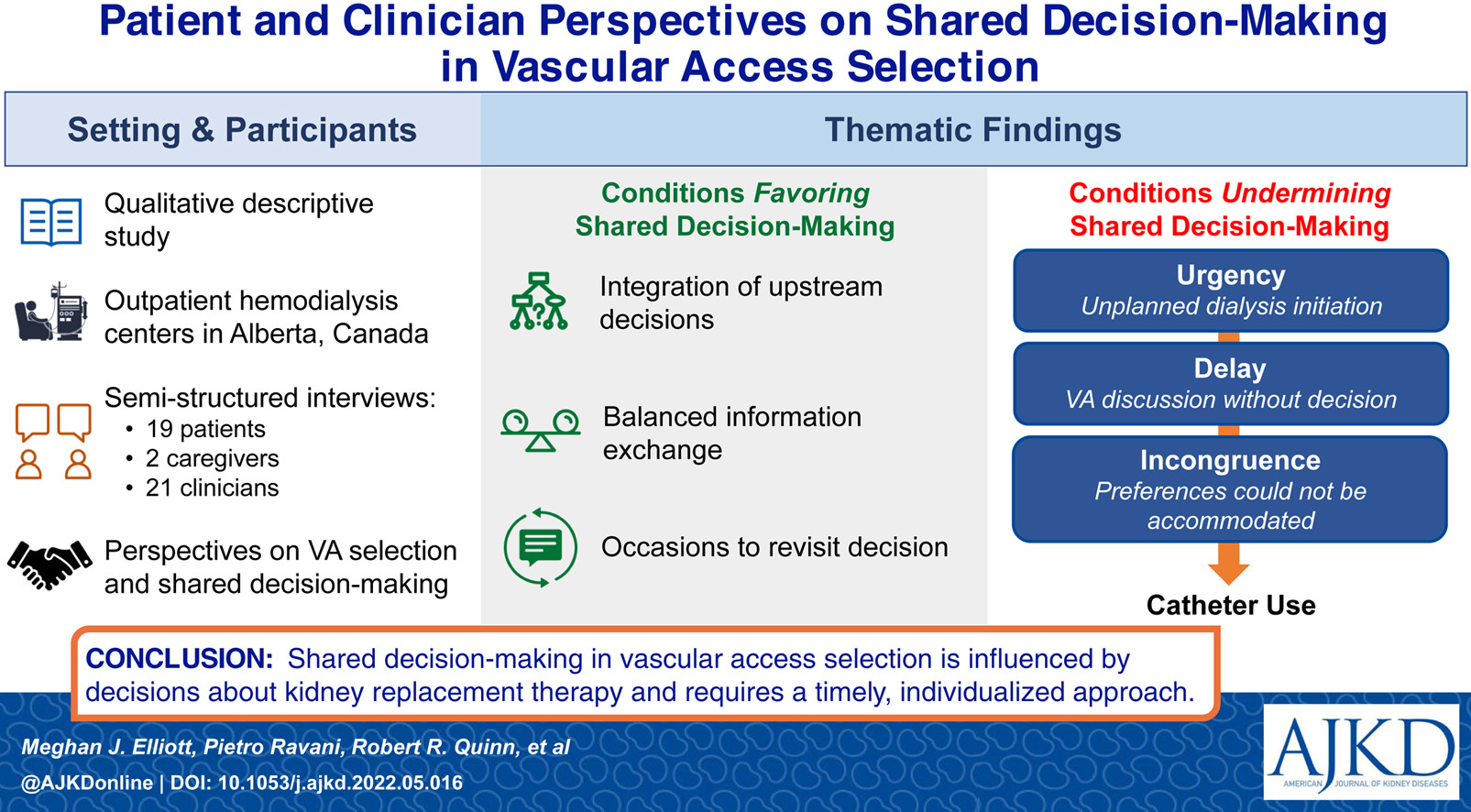
DOI: 10.1053/j.ajkd.2022.05.016
Blog Post: Hemodialysis Access Shared Decision Making by Melandrea Worsley and L. Parker Gregg [FREE]
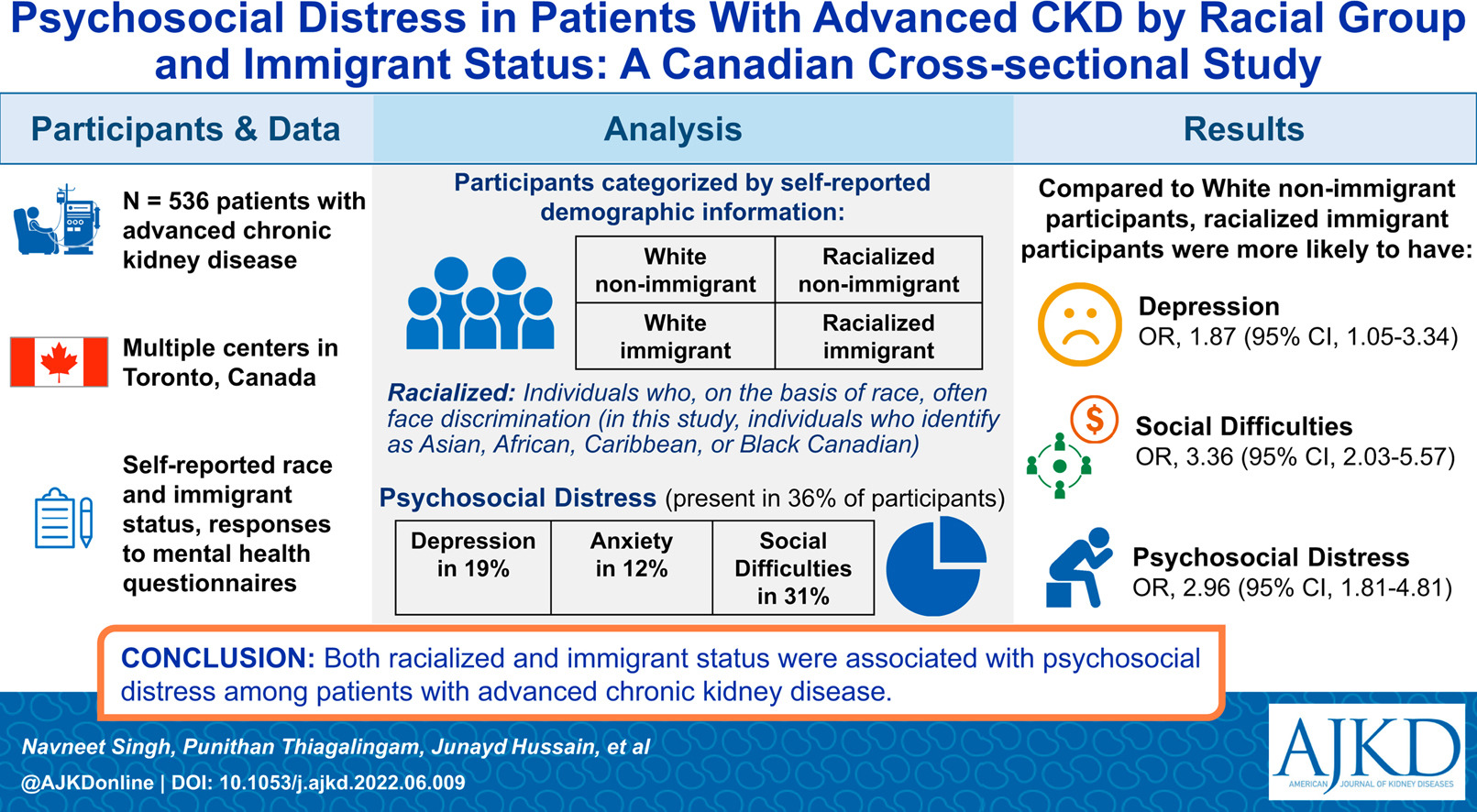
Psychosocial Distress in Patients With Advanced CKD by Racial Group and Immigrant Status: A Canadian Cross-sectional Study by Navneet Singh et al
From the authors: Psychosocial distress is frequent in patients with advanced chronic kidney disease and impacts quality of life and clinical outcomes. Psychosocial distress may be especially scarring in people who are racialized (marginalized on account of their membership in a particular racial group) and/or who are immigrants. We assessed the association of psychosocial distress with racialized and immigrant status in Canadians with advanced chronic kidney disease. Among 536 participants from multiple medical centers in Toronto, we found that racialized and immigrant participants were more likely to have psychosocial distress, depression, and social difficulties compared with White nonimmigrant participants. This is likely related to the multiple intersectional challenges, including experience with racism and discrimination that racialized immigrant patients may face. Further studies are needed to elucidate the specific factors that contribute to more distress. The potential impact of culturally competent and safe support for these patients will also need to be studied.
DOI: 10.1053/j.ajkd.2022.06.009
Review from the January 2023 issue:
Autoimmunity in Anti–Glomerular Basement Membrane Disease: A Review of Mechanisms and Prospects for Immunotherapy by Huang Kuang et al (FREE)
Anti–glomerular basement membrane (anti-GBM) disease is an organ-specific autoimmune disorder characterized by autoantibodies against the glomerular and alveolar basement membranes, leading to rapidly progressive glomerulonephritis and severe alveolar hemorrhage. The noncollagenous domain of the α3 chain of type IV collagen, α3(IV)NC1, contains the main target autoantigen in this disease. Epitope mapping studies of α3(IV)NC1 have identified several nephritogenic epitopes and critical residues that bind to autoantibodies and trigger anti-GBM disease. The discovery of novel target antigens has revealed the heterogeneous nature of this disease. In addition, both epitope spreading and mimicry have been implicated in the pathogenesis of anti-GBM disease. Epitope spreading refers to the development of autoimmunity to new autoepitopes, thus worsening disease progression, whereas epitope mimicry, which occurs via sharing of critical residues with microbial peptides, can initiate autoimmunity. An understanding of these autoimmune responses may open opportunities to explore potential new therapeutic approaches for this disease. The authors review how current advances in epitope mapping, identification of novel autoantigens, and the phenomena of epitope spreading and mimicry have heightened the understanding of autoimmunity in the pathogenesis of anti-GBM disease, and we discuss prospects for immunotherapy.
DOI: 10.1053/j.ajkd.2022.07.006
 On the Cover: The Big Dipper at Blackpool Pleasure Beach in Blackpool, England, was originally built in 1923. The second-oldest operating rollercoaster in Britain, it is 3,300 feet long and has five big drops, including twisting and banked turns. Every drop is followed by a rise to set the next drop. These drops and rises mirror the drops and rises in blood pressure that occur as part of normal diurnal blood pressure variation. In this month’s issue of AJKD, Borrelli et al report that the absence of normal nocturnal dipping is associated with higher risks of cardiovascular disease and kidney disease progression among patients with chronic kidney disease.
On the Cover: The Big Dipper at Blackpool Pleasure Beach in Blackpool, England, was originally built in 1923. The second-oldest operating rollercoaster in Britain, it is 3,300 feet long and has five big drops, including twisting and banked turns. Every drop is followed by a rise to set the next drop. These drops and rises mirror the drops and rises in blood pressure that occur as part of normal diurnal blood pressure variation. In this month’s issue of AJKD, Borrelli et al report that the absence of normal nocturnal dipping is associated with higher risks of cardiovascular disease and kidney disease progression among patients with chronic kidney disease.
The photograph “big dipper roller coaster” by Travel Stock Photos is released on Flickr under the CC BY 2.0 license



Leave a Reply